It's entirely possible, albeit rare, for patients taking antibiotics or antipsychotics to develop a sticky, black mess on top of their tongue.
Examples of the bizarre side-effect, called black hairy tongue (BHT) or lingua villosa nigra, are so few and far between that most physicians have only ever seen them in textbooks.
So when Dr Yasir Hamad at the Washington University in St Louis heard that a patient's tongue had turned black, he jumped at the chance to examine them.
It was the first case he had seen in his decade-long career.
The patient was a 55-year-old woman, who was admitted to hospital after a motor vehicle accident had crushed both of her legs. When her wounds became infected, doctors put her on an intravenous drip containing a broad-spectrum antibiotic, called minocycline.
One week on the medication was all it took. Without warning, her tongue began to turn as dark as night. She also reported feeling nauseous and said she had a bad taste in her mouth.
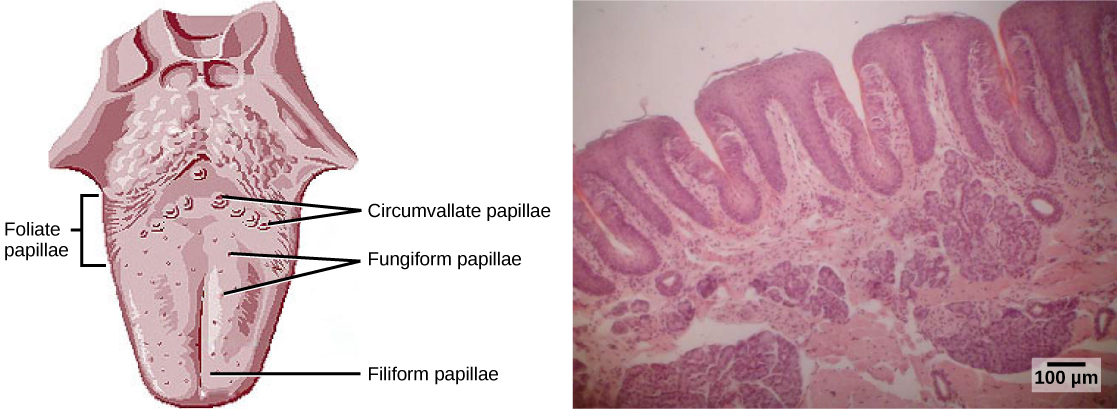
Unlike the name suggests, black hairy tongue isn't actually hair in the common sense. The term refers to the little bumps on our tongues, called filiform papillae, which contain taste buds on their upper surface.
When a patient develops black hairy tongue, these tiny knobs begin to swell in size, from around one millimetre long to as much as 18 millimetres long.
As these papillae grow, they trap minuscule bits of food between them, allowing bacteria and other microbes to fester. This is what turns the surface of the tongue brownish-black.
Warning: gross picture ahead! You have been warned.
Scientists still aren't sure why this peculiar side-effect develops, but it's not anything to stress over.
It's highly uncommon and quite harmless - although it is more likely to happen to smokers, those with specific medical conditions, those with poor oral hygiene and those who use irritating mouthwashes.
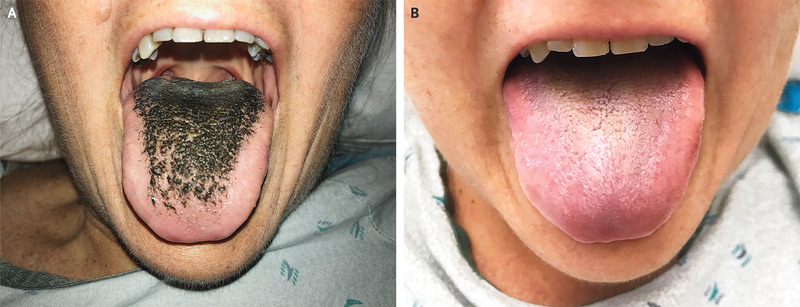 (The New England Journal of Medicine)
(The New England Journal of Medicine)
"As scary as this looks, the good part is that it's actually reversible," Hamad told CNN.
It also has no known long-term effects, and there are various ways to treat it, including increased hydration and salivation, the cessation of smoking, brushing the tongue with a soft toothbrush and applying topical retinoids or salicylic acid. In extreme cases, some physicians resort to surgical excision.
In this particular case study, all that the doctors had to do was take the patient off of the medication and place her on a different antibiotic. Within four weeks, her tongue was back to its normal colour.
"A lot of things you can diagnose just from looking at the mouth," Hamad advised other doctors.
"That's the lesson: Don't miss that part of the body when you're examining the patient".
The case study has been published in The New England Journal of Medicine.