People with blood type B may need to be a little more vigilant than their peers about the lifestyle factors associated with diabetes risk.
According to a 2024 umbrella review, people with blood type B – either positive or negative – had a slightly higher risk of developing type 2 diabetes than people with non-B blood types.
How much higher? About 28 percent, on average. That's not huge, but it may be significant enough to tip the scales if other risk factors are involved.
"Numerous systematic reviews with meta-analyses have been published, which explored correlations between ABO and Rhesus blood groups with various health outcomes.
"However, to date, the association between these blood groups and human health outcomes remains controversial," wrote a team led by epidemiologist Fang-Hua Liu of Shengjing Hospital of China Medical University.
"The current umbrella review included 51 systematic reviews with meta-analysis articles with 270 associations.
"We re-calculated each association and found only one [instance of] convincing evidence for an association between blood group B and type 2 diabetes mellitus risk compared with the non-B blood group."
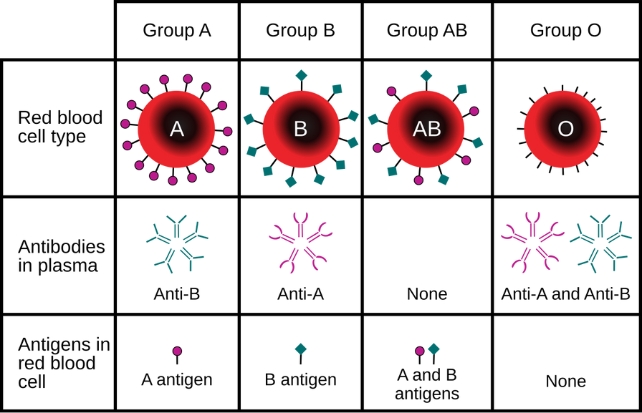
Human blood is categorized into eight main groups based on the sugars and proteins, or lack thereof, present on the surface of your red blood cells.
A, B, and AB types are based on the presence of antigens – sugar molecules that can trigger an immune response. O-type blood has no A or B antigens. Meanwhile, Rhesus (Rh) factors are proteins that determine blood compatibility and give your blood its positive or negative designation.
Previous studies have suggested that these subtle differences in our blood cells may be linked to increased vulnerability to certain diseases.
Liu and colleagues embarked on their study to systematically evaluate links between blood type and disease across a catalog of around 270 different health outcomes.
A systematic review is a study that reviews published papers on a given topic and analyzes their results collectively. An umbrella review compiles systematic reviews – a sort of giant synthesis that provides a wider overview.
Think of individual studies as trees; a systematic review is like standing outside a copse, while an umbrella review is like flying a drone over a whole forest of copses.
"We systematically searched PubMed, Web of Science, Embase, Scopus, Cochrane Library, and several regional databases on the date from inception until Feb 16, 2024, to identify systematic reviews with meta-analyses of observational studies evaluating associations between ABO as well as Rh blood groups and diverse health outcomes," the researchers explained.
To sort through the 270 reported links between blood group and disease, the researchers put each one through a series of statistical stress tests designed to weed out weak or unreliable findings.
They examined the strength of the evidence, whether results were consistent across different studies, and whether the datasets were large enough to be trustworthy. They also checked for signs of bias, such as small studies exaggerating effects or an unusually high number of positive results.
Crucially, they asked whether each association would likely hold up if tested again in future research. Most of the associations didn't pass these checks.
In the end, just one link, between blood type B and type 2 diabetes, met the highest standard of evidence.
That suggests that the link is real, albeit relatively small: just 28 percent higher than the current baseline. That's much smaller than the risk associated with diet, weight, or lifestyle.
Just 50 grams of processed meat a day, for example, increases the risk of type 2 diabetes by 37 percent. A sedentary lifestyle can increase the risk by 112 percent. And being overweight is one of the strongest risk factors known.
Related: A Distinct New Type of Diabetes Is Officially Recognized
The researchers also didn't examine what might drive this increased risk. A 2025 study suggests that the gut microbiome may be involved; however, further investigation is needed.
The results do suggest that there's a real, tangible association between blood type and type 2 diabetes – one that people can factor into how they think about their own risk.
More broadly, the study highlights weaknesses in existing research that better-designed reviews can address, and shows that more rigorous work is still needed to understand how blood type relates to disease.
The research was published in BMC Medicine.