The last time a male contraceptive was approved for use in the United States was in the 1980s.
Finally, in 2026, alternatives to condoms and vasectomies are on the horizon.
The next generation of male contraceptives is already in phase 2 human clinical trials, and now, after years of work in mice, scientists at Cornell University have discovered how to block sperm formation within the testes at a critical point.
Their newly tested contraceptive drug proved to be effective, safe, and reversible in male mice. Within six weeks of stopping the injections, normal sperm production began again, and two generations of offspring were born with no abnormalities.
"We're practically the only group that's pushing the idea that contraception targets in the testis are a feasible way to stop sperm production," says geneticist Paula Cohen from the Cornell Reproductive Sciences Center.
The team's target is a crucial process called meiosis, which takes place in mammalian testes.
Meiosis occurs after mitosis – when stem cells become sperm precursors – and involves a cell with two complete sets of chromosomes splitting into four new cells with half the chromosomes needed for life to form. Each of these matures to become a sperm cell.
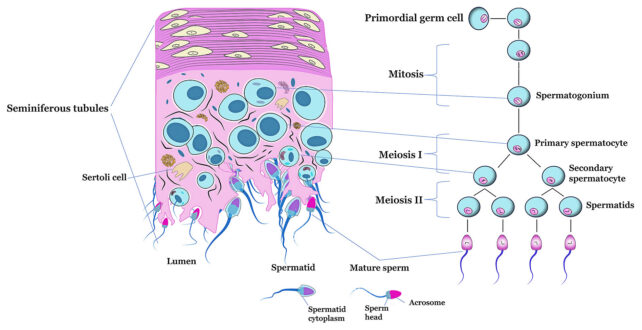
"Meiosis represents a natural checkpoint in sperm production where transient inhibition could achieve precise and reversible fertility control," argue Cohen and colleagues.
The key is to avoid killing off self-renewing stem cells before mitosis occurs, as this could lead to irreversible infertility. Once those stem cells proliferate and differentiate, however, there's a chance they could sneak out of the testis as sperm and fertilize an egg.
The drug JQ1 strikes at the perfect time. It was originally developed to stop cancerous tumors from proliferating, but it now also appears effective at preventing sperm stem cells from undergoing meiosis.
Future safety assessments are needed before research can begin in humans, but Cohen and colleagues say that their study provides "a blueprint for developing new contraceptive approaches that act safely and selectively within the germline."
Today, as it stands, male contraception is confined to vasectomies and condoms, but recent surveys suggest that male respondents are willing to try new contraceptives if given the option.
One of the worries is that the contraception will come with dangerous or unpleasant side effects. Similar to female contraception, hormonal contraceptives increase the odds of that happening.
"We were really motivated to look for nonhormonal contraceptive targets in the testis, something that stops sperm production without affecting male libido and secondary sex characteristics," explains Cohen, referring to traits that arise with puberty, such as facial and chest hair, or a deeper voice.
Related: Promising New Male Contraceptive Passes First Human Safety Trial
"Our study shows that mostly we recover normal meiosis and complete sperm function, and more importantly, that the offspring are completely normal," Cohen says.
That's promising news, but there's still a way to go before JQ1 can be tested in humans. A male contraceptive that entered a phase 2 clinical trial last year, called YCT-529, essentially stops the precursors of sperm, before meiosis. It may be on the market sooner.
"Few reversible male contraceptives have advanced toward clinical translation," the authors write.
"The development of reversible, nonhormonal male contraceptives remains a critical unmet need for achieving reproductive equity."
The study was published in the Proceedings of the National Academy of Sciences.