Defeating obesity is rarely easy. For many people, even successful weight loss is followed by a prolonged struggle to prevent the weight from coming back.
Obesity relapse is common, and research indicates it's more than a matter of willpower. Fat cells retain a 'memory' of obesity long after weight loss, studies have found, potentially undermining efforts to avoid regaining weight.
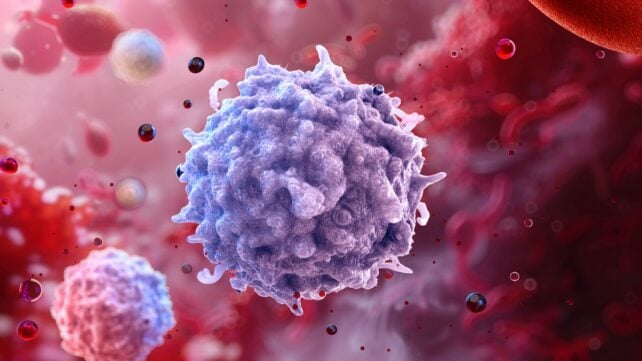
And it's not just fat cells. As researchers report in a new decade-long study, certain immune cells can also carry a persistent memory of obesity.
This record can preserve an elevated risk of obesity-related illness, the study suggests, up to 10 years after a person slims down.
The mechanism for this is DNA methylation, a normal biological process in which methyl groups latch onto DNA molecules, altering gene activity without disrupting the DNA sequence.
In people who have recently recovered from obesity, specific additions to the DNA in helper T cells seem to preserve the cellular memory of being obese, promoting a dysregulated, pro-inflammatory condition that can endure for years despite reductions in body weight.
To determine this, researchers analyzed immune cells from several groups of human subjects. These included samples from patients with obesity who either exercised four times a week for 10 weeks or received injections of semaglutide for weight loss, along with control groups.
They additionally studied samples from people with Alström syndrome, a rare genetic disorder that tends to involve childhood obesity, and from healthy matched pairs as controls.
The researchers also investigated the mechanics of obesity's lasting influence on immune function by analyzing the immune cells of mice that were fed high-fat diets, as well as blood donations from human volunteers.
"The findings suggest that short-term weight loss may not immediately reduce the risk of some disease conditions associated with obesity, including type 2 diabetes and some cancers," says co-lead author Claudio Mauro, an immunologist at the University of Birmingham in the UK.
"Instead, ongoing weight management following loss will see the 'obesity memory' slowly fade," Mauro says.
"This may take several years of sustained weight loss maintenance, likely five to 10 years, though this requires further study, to fully reverse the effects of obesity on T cells."
These discoveries shed light on the immune system's record-keeping habits, says senior author and molecular epidemiologist Belinda Nedjai from Queen Mary University London.
"Our findings show that obesity is associated with durable epigenetic modifications that influence immune cell behavior," Nedjai says.
"This suggests that the immune system retains a molecular record of past metabolic exposures, which may have implications for long-term disease risk and recovery."
In people with obesity, helper T cells 'memorize' obesity and promote weight regain, as previous research has shown. The mechanism for this has remained unclear, however.
The new study identifies two key cell functions as pathways for obesity-related methylation to influence helper T cells: autophagy, the natural removal and recycling of cellular waste, and immune senescence, or aging of cells in the immune system.
DNA methylation from obesity seems to affect both functions, a crucial insight about the prevalence and underpinnings of relapse, says co-author and immunologist Andy Hogan from Maynooth University in Ireland.
Related: Just 5 Days of Junk Food Can Trigger Obesity's Hold on Your Brain
"We know obesity is a chronic progressive and relapsing disease, and our findings provide further understanding of exactly what are the molecular mechanisms potentially driving the risk of relapsing, and highlight the challenges facing people living with obesity to successfully manage their weight," he says.
These findings could also help set the stage for targeted treatments that, along with other interventions, reverse the effects of obesity on T cells.
"Our study suggests potential therapeutic opportunities to expedite this process, such as repurposing drugs like SGLT2 inhibitors, which have shown promise in reducing inflammation and promoting immune-mediated clearance of senescent cells in obesity," Mauro says.
The study was published in EMBO Reports.