First, it was named after two men. Then, it was named for a false premise.
At last, after more than a century, one of the most prevalent hormone disorders in the world has a title that is no longer inaccurate, misleading, or outdated.
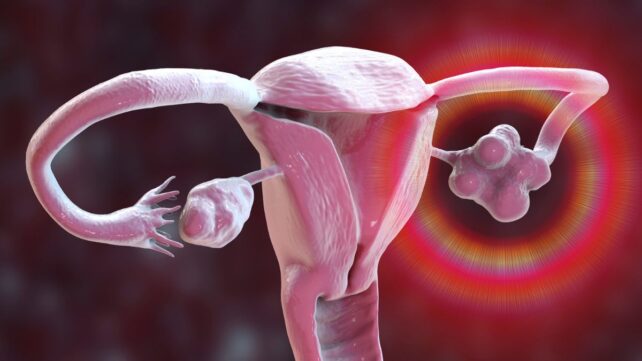
Polycystic ovary syndrome (PCOS) should now be known as polyendocrine metabolic ovarian syndrome (PMOS), according to a global science consortium.
The new name was announced this week at the European Congress of Endocrinology in Prague, after 14 years of collaboration between healthcare experts, patients, and advocates.
"The term polycystic ovary syndrome (PCOS) has long been recognized as inaccurate and potentially harmful," write the team behind the initiative, led by Verity, a UK-based charity, Australia's Monash University, and the international organization Androgen Excess and PCOS Society.
"The current name reflects only one organ and fails to capture the disorder's multisystem nature."
Lorna Berry, a patient with PMOS who worked on the initiative, said last year that she hoped the change would lead to "better outcomes for women with PCOS across their lifetime".
"For decades, those of us living with this condition have had to 'fight' for diagnosis, and even after diagnosis, misinformation is abundant," Lorna said.
One of the biggest misconceptions is that PMOS is solely a reproductive disorder, which begins in the ovaries. While infertility may be a struggle for some patients, that is not always the case, and the effects of this syndrome extend far beyond the ovaries, maybe even starting in the brain.
While PMOS can lead to irregular menstrual periods, abnormal ovulation, excess facial or body hair, acne, and sometimes infertility, it is also associated with significant endocrine, metabolic, psychological, and dermatological symptoms.
These can persist far beyond a person's reproductive years.
Today, PMOS impacts roughly 170 million people worldwide, and it's estimated that up to 70 percent of patients go undiagnosed.
The name may be part of the reason why.
The most obvious change between PCOS and PMOS is the removal of the 'C' for 'cystic'. (The terms will remain interchangeable for the next three years, per the consortium.)
The 'cysts' behind polycystic ovary syndrome first received widespread attention when they were described by two Chicago surgeons in 1935.
Irving Stein and Michael Leventhal were investigating infertility in women, and they noticed during surgery that their patients' ovaries were enlarged and contained numerous small, cyst-like structures.
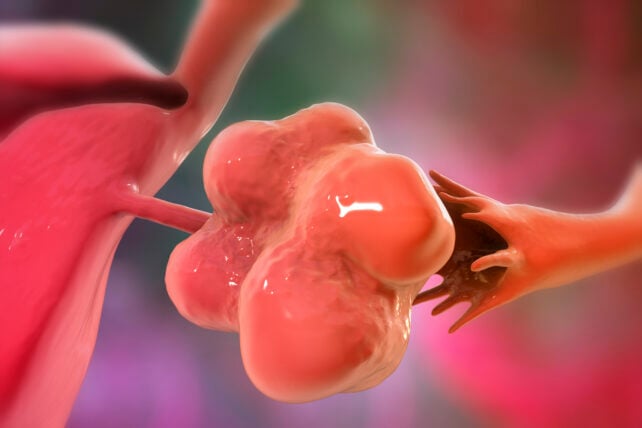
When the surgeons removed these 'cysts', they reported that menstrual cycles resumed, and some patients went on to have biological children of their own.
At the time, scientists were just beginning to understand how the female body ovulates. Sex hormones like estrogen and progesterone had only recently been discovered.
In 1958, decades after that first discovery, Stein published an article in which he called the diagnosis the Stein-Leventhal Syndrome and claimed it could be cured with surgery.
Later, the syndrome would become widely known as PCOS.
These 'cysts', however, would turn out to be something else entirely: ovarian follicles that had stopped growing. Today, we know that these underdeveloped eggs aren't a unique feature of PMOS, and they rarely require surgical removal.
In fact, some patients with PMOS don't even show evidence of these immature eggs in ultrasounds.
Terhi Piltonen is an obstetrician and gynecologist in Finland who is involved in the global name change policy. She recently told ABC News Australia that the term PCOS is "confusing".
"Many women, and even professionals, believe the PCOS ovary contains large cysts that can burst or require surgical treatment, whereas the truth is that the ovary is 'full and lush' and has a high reserve of small underdeveloped follicles with oocytes [eggs]," she told health reporter Lauren Roberts.
"So the ovarian focus has done harm in the sense that many women have been ignored with their symptoms related to weight and other metabolic problems, mental distress, and skin manifestations."
There is still no known cause or cure for the syndrome, and treatments vary widely among individuals, but hormonal, metabolic, and surgical options are currently available to improve quality of life.
Many patients, however, are not receiving prompt diagnosis or proper care.
Adding the term 'metabolic' to the name could help. Today, it is estimated that as many as 85 percent of patients with PMOS suffer from insulin resistance, and they also face a higher risk for type 2 diabetes, obesity, and fatty liver disease.
Yet they are often not screened properly for these conditions.
In 2023, endocrinologist Blazej Meczekalski from Poznan University in Poland penned an editorial that argued the term PCOS is "misleading, confusing, and generally [projects] a negative image onto patients."
From 1935 to the end of the 1970s, he explains, research was mostly focused on the hormonal aspects of PCOS. In the last two decades of the 20th century, however, the focus shifted to metabolic issues involving hormones such as insulin.
In the year 2000, one of the first randomized, double-blind, placebo-controlled studies was published investigating whether the diabetes medication metformin could be used to treat symptoms of PMOS.
The results were highly encouraging. Metformin significantly reduced circulating levels of insulin, which relate to insulin resistance, and circulating levels of testosterone.
Since then, research has increased exponentially, and yet drugs like metformin are still often prescribed 'off-label' for PMOS. This means they aren't officially approved forms of treatment, paid for by insurance agencies or governments.
These drugs can cost hundreds of dollars a month out of pocket for patients who live in the US, for example.
Perhaps the 'metabolic' in PMOS will help steer drug researchers, insurance companies, government agencies, physicians, and patients in the right direction for optimal care.
Related: Having Both Ovaries Removed Could Come at a Serious Cost to The Brain
Over the next three years, the strategy is to educate the global public on PMOS and convince international classification bodies to transition away from using the term PCOS.
Ultimately, the goal is for the World Health Organization (WHO) to update the term PMOS in its International Classification of Diseases (ICD), which 195 nations currently follow.
The argument for PMOS and its implementation strategy are outlined in a health policy paper for The Lancet.