The University of Oxford has just launched a Phase 1 trial to test a new vaccine against a very old enemy – plague – all based on technology that is helping humanity fight COVID.
And they want you to help: They're recruiting for volunteers who are happy to be jabbed in the name of science to test a new experimental vaccine.
While infamous for its historic outbreaks like the Black Death that swiftly killed around half of Europe's population in the 1300s, plague still ravages parts of Africa and occasionally breaks out elsewhere too. Only last week, a 10-year-old boy died of complications from plague in the US.
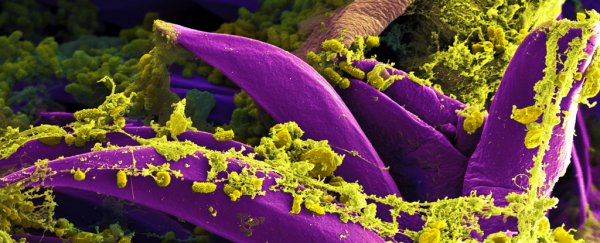
Caused by the bacteria Yersinia pestis, plague can be transferred from animals to humans via fleas, and then spreads through contaminated body fluids or other materials. Untreated, this horrific disease can be rapidly fatal, with as much as a 100 percent mortality rate depending on how it infects the body.
It can begin with flu-like symptoms – fevers, chills, aches, and fatigue – and in its most common form progresses to inflamed and painful lymph nodes, which are called buboes. This is where the term bubonic plague comes from.
If the bacteria multiply in your bloodstream, it causes septicemic plague, which can include vomiting, diarrhea, bleeding, and gangrene.
The least common form of plague is pneumonic plague, when Y. pestis infiltrates your lungs, the most dangerous form of the infection, which can progress to rapid respiratory failure and shock within two days of infection.
The number of plague cases has increased in 25 countries since the 1990s. Globally 3,248 cases, including 584 deaths, were reported between 2010 and 2015. The 2017 outbreak in Madagascar caused 2,119 confirmed and suspected cases, including 171 deaths.
The most effective way to treat plague is through the use of antibiotics, so a quick diagnosis is critical – particularly for the pneumonic form. Unfortunately, this is not always possible.
"Although antibiotics can be used to treat plague, many areas experiencing outbreaks are very remote locations," explained vaccinologist Christine Rollier from the University of Oxford.
"In such areas, an effective vaccine could offer a successful prevention strategy to combat the disease."
The Oxford Vaccine Group has developed an intramuscular vaccine using a modified cold virus (adenovirus) that can't multiply in humans, similar to the one used in the AstraZeneca COVID-19 shot.
The virus will be used to deliver the gene code for a protein from Y. pestis that is essential to its ability to infect us, in order to teach our immune system to recognize it as an invader – just like how many COVID-19 vaccines target its spike protein.
So far, the plague vaccine has only been tested on laboratory animals, but with promising results.
As with any vaccine, side effects could range from localized pain to more severe but rare allergic reactions, but all participants in the clinical trial will be closely monitored – particularly during the first week after the vaccination.
Most side effects should be temporary, but in "rare cases, side effects can be serious or prolonged, although no serious concerns have been raised in human trials for other similar virus-based vaccines," the research team explains in the Study Information Booklet.
In this booklet, the team also addresses the possibility of the rare blood clots that have been reported in connection to the AstraZeneca coronavirus vaccine.
The situation is being closely monitored by health authorities worldwide, but it appears to occur in five out of a million people who receive the vaccine. It is not known if this is connected to the coronavirus part of the vaccine, or another part of the ingredients – but the team notes no other clinical trials using this vaccine method have resulted in blood clots.
The team are looking for healthy people between 18 to 55 to participate in the year-long study, and are offering £630 (about US$880) to those who are recruited to take part.