The natural removal of toxic proteins that clump together in the brain to cause Alzheimer's disease and other neurodegenerative disorders can be boosted by a drug that increases activity in the brain's 'garbage disposal', according to a new study.
Neuroscientists at Columbia University Medical Centre (CUMC) say that rolipram, a discontinued medication that was developed for its potential use in treating depression, can boost activity in the brain's proteasome system, which grinds up old proteins so they can be recycled into new ones.
"We have shown for the first time that it's possible to use a drug to activate this disposal system in neurons and effectively slow down disease," said lead researcher Karen E. Duff. "This has the potential to open up new avenues of treatment for Alzheimer's and many other neurodegenerative diseases."
Brain cells naturally clear out old or damaged proteins as part of their regular maintenance thanks to proteasomes, which are shaped like small molecular cylinders. However, sticky proteins like amyloid beta and tau proteins that contribute to the development of Alzheimer's disease impede this normal garbage disposal system, clumping together and resisting efforts to remove them.
In the study, which is reported in Nature Medicine, the researchers used a mouse model of neurodegeneration and found that tau proteins accumulate by sticking to the proteasome and slowing down the usual protein disposal process.
However, administering rolipram reactivates the proteasome and restores a normal level of protein removal. In diseased mice, the researchers found that the drug also improved memory levels to those seen in healthy mice.
Rolipram is able to do this by inhibiting an enzyme called PDE–4, and while the researchers don't fully understand how it works, the inhibition of the enzyme results in increased proteasome activity.
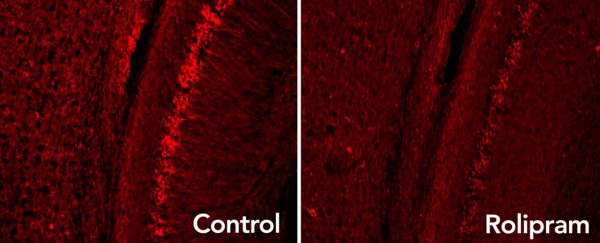
You can see the results in the images above, with the rolipram on the right having eliminated excess tau proteins (the bright red dots, seen in far greater number on the left image).
"We still don't know exactly where the activation is happening, but what's new is that we can modify the proteasome to increase its activity. There could be many other ways to do this," said one of the team, Natura Myeku.
And that's fortunate, because rolipram itself isn't particularly suitable for use in humans, as one of its side effects is inducing nausea. Luckily, the researchers say similar proteasome-targeting drugs also exist and don't carry such side effects, and they could go into clinical trials relatively quickly.
If such drugs are shown to be safe and to work in people like they do in mice, they could work as a kind of silver bullet to help us treat Alzheimer's and other diseases caused by the accumulation of abnormal proteins, such as Parkinson's, Huntington's, and frontotemperoral dementia.
"Treatments that speed up these cell disposal mechanisms should, in theory, only degrade abnormal proteins. We don't need to know what the toxic form of the protein is," said Duff. "In Alzheimer's disease, there are at least four different types: amyloid, tau, alpha-synuclein, and TDP43. A well-functioning proteasome can clear out everything at once."