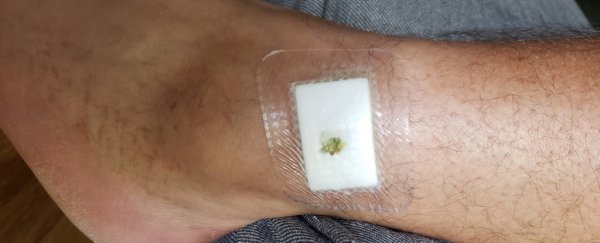
Eight months after his last trip to our grandparents' beach house, my brother Alex was diagnosed with a flesh-eating bacterial infection related to leprosy and tuberculosis. And it's becoming more common.
We've been holidaying down at the beautiful Mornington Peninsula since we were kids. There, we've experienced the typical childhood scrapes and bruises, mosquito and sandfly bites, and the occasional sunburn - but never anything like this before.
"I didn't notice anything until I accidentally scratched myself on the leg about six months after I was away," Alex said. "It looked like I'd punctured my skin.
"I didn't think much of it at the time, but then a month later it still hadn't closed and it was starting to ooze puss." (WARNING: photo of the wound further down.)
At first, his doctor simply treated him for a regular bacterial infection, and sent off samples for testing.
"When the first lot of tests came up empty, my doctor had a hunch, and tested specifically for the Buruli ulcer."
This test verified he was being eaten by Buruli ulcer bacteria (Mycobacterium ulcerans), also known locally as the Bairnsdale ulcer. So, Alex was referred to a specialist at Victorian Infectious Disease Services (VIDS).
M. ulcerans infection lies dormant two to nine months between exposure and appearance of symptoms. Thankfully, it is not known to spread between people.
The infection occurs across 33 countries, most commonly affecting rural Africans with little access to health care. This and the fact that we still don't know many basic things about it, has earned it the classification of "neglected tropical disease" by the World Health Organisation.
"We are not sure exactly how people are contracting this disease," explains CSIRO virologist Kim Blasdell. "However, a recent study has suggested that if the bacteria ends up on the surface of someone's skin… and they then suffer a puncturing injury such as a mosquito bite or thorn prick, then the infection can develop at this site."
"M. ulcerans has been detected in both soil and water. It's also been found in a range of native and introduced mammal species, and in a variety of arthropods including aquatic insects and mosquitoes," Blasdell told me.
One of the oddest things about this infection is that although Alex's wound looked sickeningly gross and horribly painful, his leg felt just fine.
"Most of the time I couldn't feel anything," he said. "I only remember the pain when I scratched my leg and then it started to hurt a bit soon after the antibiotics - a distant irregular ache."
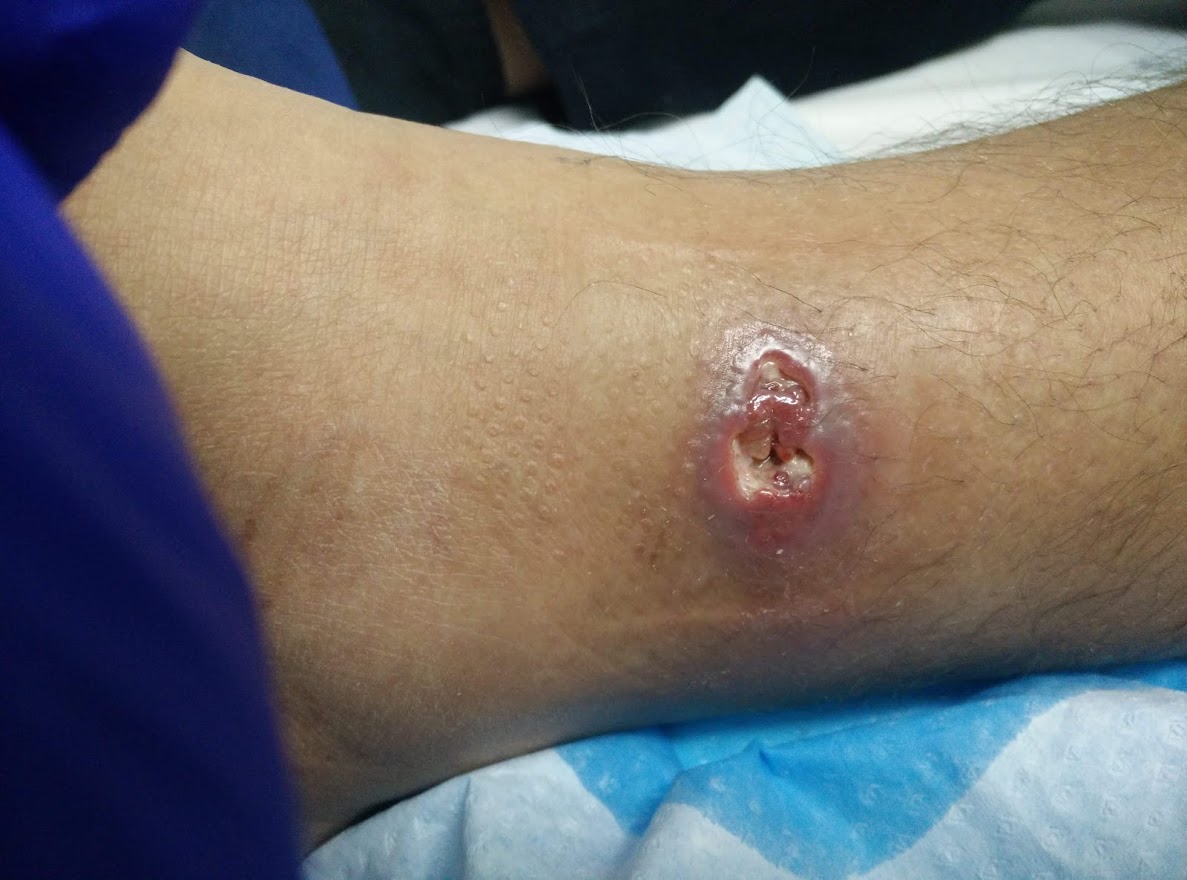 Alex's leg soon after starting treatment for the Buruli ulcer infection. (Tessa Koumoundouros)
Alex's leg soon after starting treatment for the Buruli ulcer infection. (Tessa Koumoundouros)
According to University of Melbourne's infectious diseases specialist Daniel O'Brien, that's because the bacterium produces a toxin that not only dissolves flesh, but also numbs the pain.
"It produces an anaesthetic agent so a lot of the time, especially early on, patients don't feel it," he told the ABC, and "it actually paralyses the immune system."
A 2008 study of the Buruli ulcer identified a toxin called mycolactone as the cause of nerve damage in mice - cutting off the pain from detection by the brain. More recent research has untangled how this toxin subdues the immune system. This trait makes it easier for people to ignore the problem far longer than they probably should.
Soon after Alex's diagnosis, we noticed reports of increasing incidents of Buruli ulcer in the local news.
"The number of cases and distribution of the disease have increased in recent years and it is not yet understood why," said Blasdell.
One of the specialists Alex spoke to mentioned that warmer weather might have something to do with this increase. Medical specialists have long been warning about the potential for climate-change-fuelled heat to spread diseases.
Most infectious hotspots are in the tropics, not temperate locations like Mornington Peninsula, in the Australian state of Victoria. But Blasdell explained that the Buruli ulcer has been found in other temperate regions, such as Japan.
"This suggests factors other than just temperature likely determine its distribution," she told me.
Blasdell and her colleagues across multiple organisations are conducting a large-scale study to try and fill in some of these knowledge gaps, including behavioural risk factors and those to do with climate.
Alex participated in the study, answering questions and arranging access to my grandparent's property for the researchers. There, the scientists collected soil samples and rigged sticky mozzie traps around the yard in an attempt to catch the infection-carrying culprits.
Fieldwork, of course, typically has some setbacks - here's what happened to one of the mozzie traps:

Despite the efforts of my cousin's mischievous young pup Bentley, the researchers were able to retrieve most of the traps, and there will be plenty more to collect.
"We are still in the early stages of this project, with the case control study expected to run for at least another 15 months," Blasdell explained. She hopes to conduct more work in the future, to find out whether some people are more susceptible, and how symptoms develop in different people.
Meanwhile, catching this nasty infection can require some pretty intensive treatment.
"I had to take two types of antibiotics for eight weeks," Alex said. "It gave me digestive issues - including piss that looked like orange-flavoured Gatorade."
On researching this story, we found Alex actually got lucky. In his article for The Conversation, O'Brien pointed out that while the treatment is almost 100 percent effective, almost a quarter of people can react badly to the antibiotics used.
Even worse, if the wound is allowed to get too big, patients can end up needing plastic surgery, or in most extreme cases it can lead to amputations and other deformities.
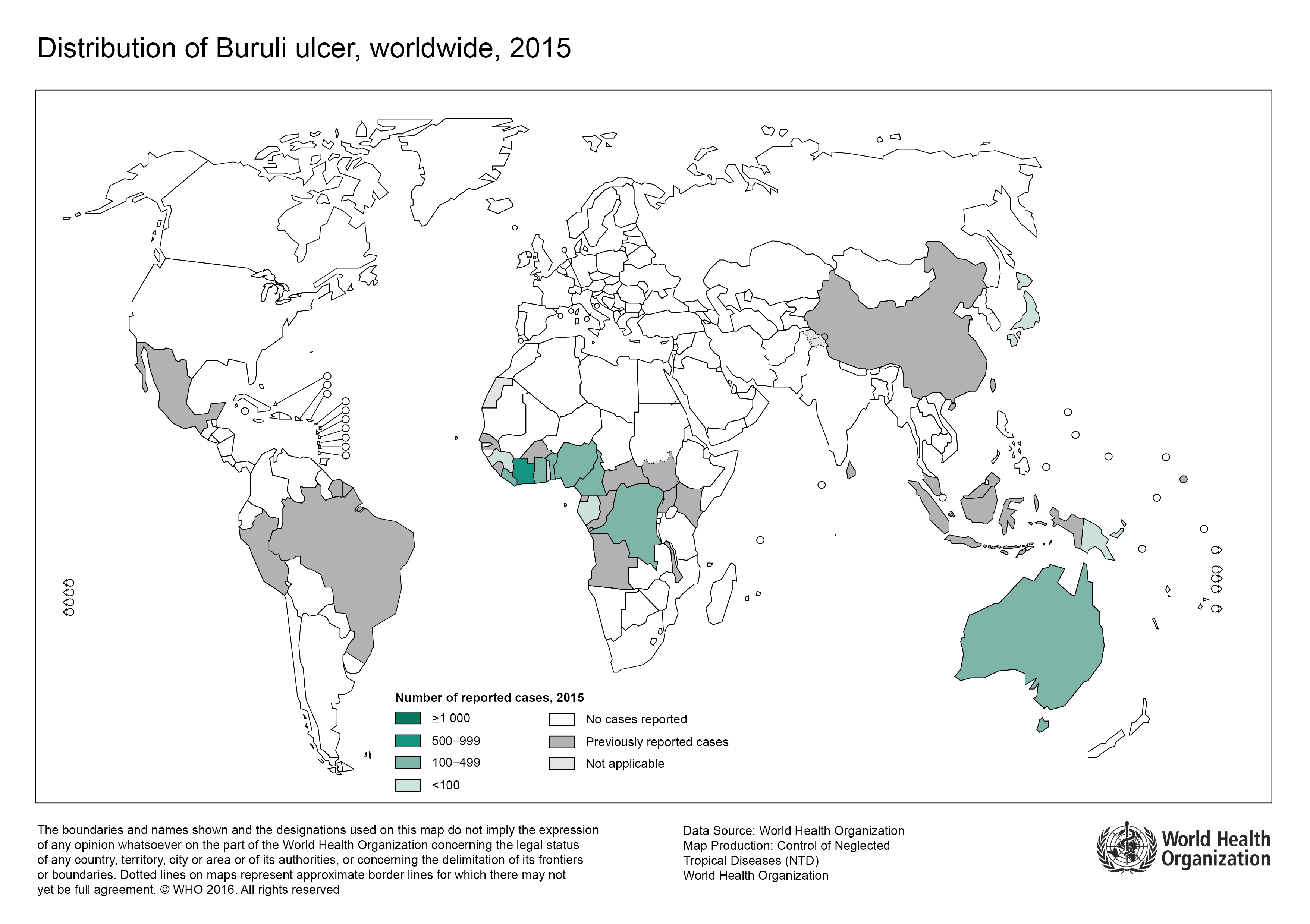 Buruli ulcer distribution in 2015 (WHO)
Buruli ulcer distribution in 2015 (WHO)
So, if you've been to any of the areas in the map above and notice a peculiarly persistent yet painless lump or wound, learn from my brother's experience and get it checked by a doctor sooner rather than later.