Pushing the body towards ultra-marathon distances can cause red blood cells to be less flexible, potentially impacting their ability to deliver oxygen and remove waste throughout the body, a new study shows.
Although the study didn't look at long-term health implications, there are reasons to believe that hitting our biological limits in this way may be harmful – something that has been hinted at by earlier research.
The international team of researchers behind the new study think it might be a stress and repair problem: that the pressures of running ultra-marathon distances exceed our innate recovery abilities.
This is something red blood cells are particularly vulnerable to, as they lack a nucleus and can't repair themselves by making new proteins. However, the researchers stop short of recommending against taking part in these runs.
"We don't have guidance as to whether people should or should not participate in these types of events," says biochemist and molecular geneticist Travis Nemkov, from the University of Colorado Anschutz (CU Anschutz) in the US.
"What we can say is, when they do, that persistent stress is damaging the most abundant cell in the body."
The study involved 23 elite runners competing in either the Martigny-Combes à Chamonix race (40 kilometers or about 25 miles – slightly shorter than a marathon) and the Ultra Trail deMont Blanc race (171 kilometers or about 106 miles long – an ultra-marathon).
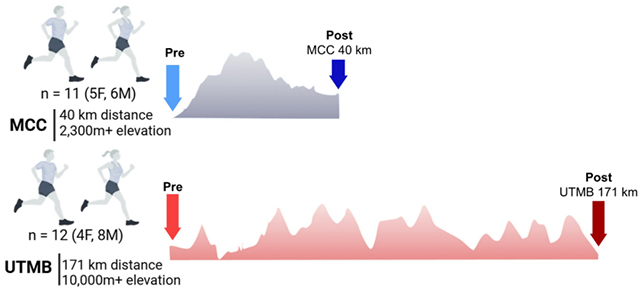
Nemkov and colleagues measured levels of a host of different biomarkers in blood samples collected from athletes before and immediately after the race.
As expected, red blood cells showed damage from a variety of causes, including mechanical (from physical strain) and molecular (from internal chemical changes).
Generally, these signs of damage are associated with the faster aging and breakdown of red blood cells. However, the wear and tear on those cells was notably greater in those runners who completed the longer distance.
One of the significant changes was red blood cells becoming more inflexible. That potentially limits their ability to get around the body and can lead to a drop in blood cells as stiffer ones are cleared out – and this was observed only in the ultra-marathon runners.
Another difference at the longer distance was that one of the red blood cell repair strategies, known as the Lands cycle, went into overdrive – with chemical markers indicating it couldn't keep up with the body's demands.
"At some point between marathon and ultra-marathon distances, the damage really starts to take hold," says Nemkov.
"We've observed this damage happening, but we don't know how long it takes for the body to repair that damage, if that damage has a long-term impact, and whether that impact is good or bad."
As ever, it's important to give context around the results: This is a relatively small sample of runners, and there were other differences between the two race types besides length (including pace, elevation, and conditions).
That means there's no proof of direct cause and effect here, and any conclusions have to be balanced against other research. It's previously been found, for example, that elite runners tend to have significantly longer lives than the rest of us.
Future research will be able to take a look at these blood changes in larger groups of people over a longer period of time, but there's an interesting tangential finding of the study, too: The damage shown here is similar to the damage seen when blood is stored for transfusions.
Related: It Turns Out That Everything We Know About The Runner's High Could Be Wrong
Red blood cells in storage show the same sort of 'lesions' seen in the ultra-marathon runners, and the researchers suggest that these extreme running events could be used to investigate ways to improve how blood is stored for medical use.
"This study shows that extreme endurance exercise pushes red blood cells toward accelerated aging through mechanisms that mirror what we observe during blood storage," says biochemist and molecular biologist Angelo D'Alessandro, from CU Anschutz.
"Understanding these shared pathways gives us a unique opportunity to learn how to better protect blood cell function both in athletes and in transfusion medicine."
The research has been published in Blood Red Cells & Iron.

