Chemotherapy and radiation have saved the lives of millions of children worldwide, but these intense therapies also leave young patients with a substantial risk of infertility later in adulthood.
Roughly one-third of men who receive gonadotoxic treatment such as chemotherapy or radiation in childhood are deemed 'azoospermic' after puberty. That means their ejaculate lacks any viable sperm.
Now, in a world first, a medical team at the University Hospital Brussels and the Free University of Brussels (VUB) claims to have restored the sperm production of one such patient.
In a new case study, provided ahead of peer review, the team explains how they treated a male patient with no viable sperm by re-transplanting a sample of his own childhood testicular tissue into his adult testicle.
The anonymous patient was born with sickle cell anemia – an inherited blood disease that can be managed with donated bone marrow and small doses of chemotherapy in a similar way to a type of leukemia.
In 2008, before undergoing treatment, this patient (roughly age 10) and his family consented to the removal of one of his testicles, so that it might be frozen for future use.
In 2022, the anonymous man returned to Brussels IVF at VUB with the wish to have a child. However, it was found that he had no viable sperm in his remaining testicle. He requested transplantation, using the testicular tissue he had elected to freeze in childhood.
In 2025, as part of a clinical trial, the patient underwent surgery to reintroduce four tissue grafts within his testicle and four within his scrotum.
Now, a year later, some of these grafts are producing mature and motile sperm.
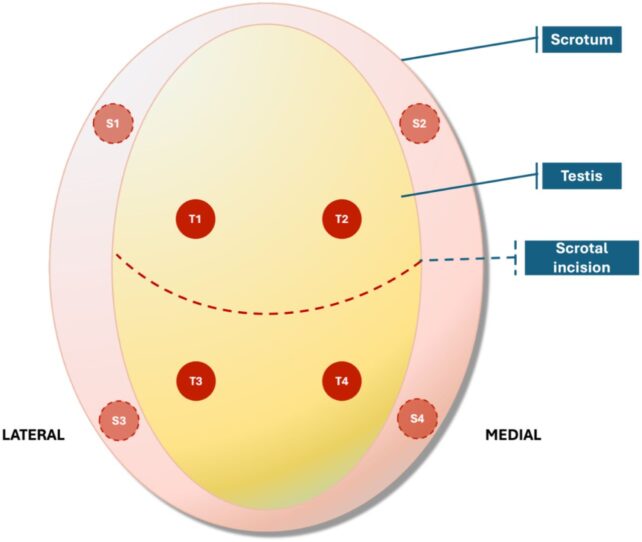
Only the parts of the testicle that contain the transplanted grafts hold viable sperm, and these are not connected to the patient's sperm duct. This means that the sperm are likely not reaching his semen.
If the patient wishes to have a child, he will probably need to undergo special treatments that carefully combine sperm and eggs in the lab.
But the possibility of becoming a parent exists where it once did not.
While the case study needs to be reviewed by independent experts, pediatric endocrinologist Rod Mitchell, who runs a similar trial at the University of Edinburgh in Scotland, says he always suspected the procedure would work.
"If you freeze tissue and keep cells alive, then they should have the potential," Mitchell told The Guardian's Hannah Devlin.
"You're putting the tissue back into the perfect environment to stimulate it. Scientifically and biologically, it makes sense. In reality, it's still amazing."
For adults who undergo chemotherapy or radiation, conventional sperm banking is typically advised. But before puberty, patients are not eligible to freeze their sperm, as the body is not producing mature versions yet.
Even in childhood, however, the testicles contain important players called spermatogonial stem cells (SSCs), which have the potential to become sperm later in life. Freezing this tissue may, therefore, be a way to preserve fertility for young patients at risk.
In 2002, the University Hospital Brussels became the first hospital in the world to introduce the practice of freezing immature testicular tissue in the hopes of preserving future fertility. In the years since, other hospitals have followed suit, providing cryopreservation for over 3,000 boys globally, and counting.
These samples were banked to enable research and in case future studies show the approach is viable. For many patients, this is the only option for fertility restoration they have.
While a single patient is not enough to prove the procedure works, the case study from Brussels provides hope that frozen germ cells can survive freezing, thawing, and grafting.
The patient's cryopreserved, immature testicular tissue showed "exceptionally low number of SSCs", and yet even that tiny fraction of cells was enough to trigger sperm production after re-transplantation.
Whether these grafts last longer than a year remains unknown. Evidence from animals suggests they may have short lifespans.
Then, of course, there's the all-important question of whether these sperm can lead to healthy babies.
"This is an important step in further scientific research to preserve the fertility of children with cancer or other blood diseases for the future," said fertility specialist Veerle Vloeberghs at Brussels IVF, after last year's successful transplantation.
"While the procedure is specifically designed to restore fertility, we cannot at this time guarantee that it will be successful or that patients can go on to have children. This treatment offers lots of perspectives for these young adults. They now have options that they did not have until recently."
Related: Humans And Animals Are Facing a Hidden Fertility Crisis, Scientists Warn
Researchers are going to keep a close eye on the patient who received this novel testicular transplant as he pursues biological parenthood.
They intend to monitor embryo development, pregnancy progression, and long-term health outcomes in any resulting offspring.
The patient's story will be watched with hope by millions.
The study is available in medRxiv.