Implants made from pig skin have restored sight to 20 people with diseased corneas, in an exciting pilot clinical trial. Many of the patients were blind before receiving the help of this bioengineered tissue.
Incredibly, after two years, all 14 of those blind people had their vision restored and three of them, and three of them now have perfect 20/20 vision.
"This gets us around the problem of [a] shortage of donated corneal tissue and access to other treatments for eye diseases," says Linköping University ophthalmology researcher Neil Lagali.
While around 12.7 million people suffer vision loss due to problems with their corneas, only 1 in 70 manage to receive a cornea transplant – the only way to restore their vision.
As the means to provide these transplants are costly, and donated corneas are in short supply, most people in the world do not have access to effective treatments.
"We've made significant efforts to ensure that our invention will be widely available and affordable by all and not just by the wealthy. That's why this technology can be used in all parts of the world," says Linköping University biomedical engineer Mehrdad Rafat.
To achieve this, Rafat and colleagues developed a new technique that requires no stitches so doctors can perform the implant procedure with less specialized conditions and equipment.
"A less invasive method could be used in more hospitals, thereby helping more people. With our method, the surgeon doesn't need to remove the patient's own tissue. Instead, a small incision is made, through which the implant is inserted into the existing cornea," explains Lagali.
What's more, the material used to create the implant is a byproduct of the food industry and, thanks to specially developed packaging and sterilization processes, the final product can be stored for up to two years. In contrast, donated human corneas must be used within two weeks.
Our cornea – the clear screen over the front part of our eye that shields our iris and pupil – is mostly composed of different types of collagen. This structure can gradually thin out over time, causing it to bulge outwards and distort our vision in a condition called keratoconus.
While the exact cause of this thinning isn't known, genetics, vigorous eye rubbing, and conditions including hay fever, asthma, Down syndrome, and Ehlers-Danlos syndrome can increase the chances of developing keratoconus.
So the researchers purified collagen from pig skin to create a new cornea layer. They used chemical and photochemical methods to strengthen this usually soft material, making it more stable, resulting in a hydrogel they've called a bioengineered porcine construct, double crosslinked (BPCDX).
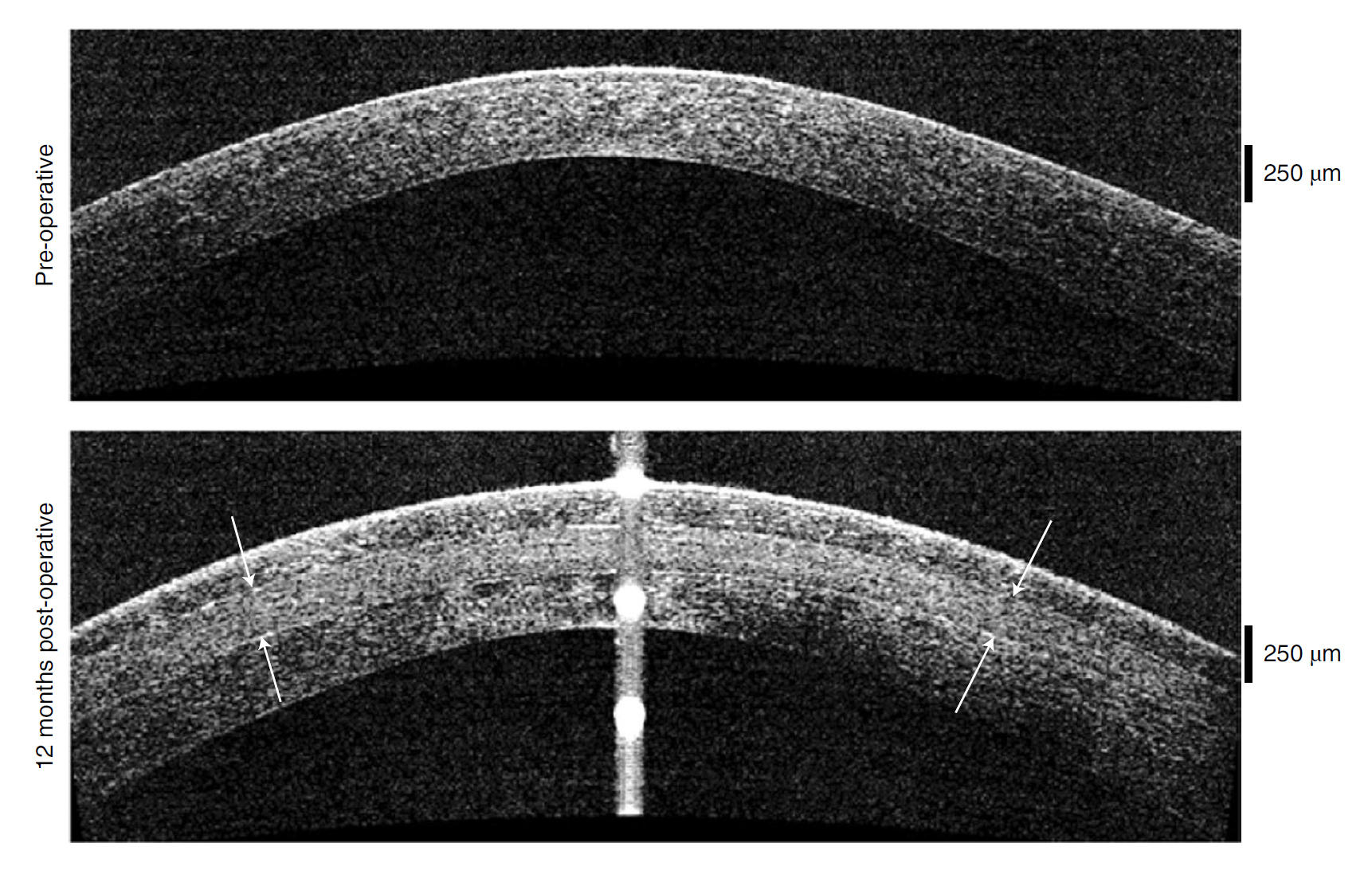
Refining their techniques in animal models, researchers then developed a simple method to insert BPCDX into the recipient's cornea, eliminating the need to remove the existing tissue.
Here, the implant flattens the cornea's buckling and provides the lost thickness, repairing the eye's capacity to focus.
The minimally invasive surgery leaves the corneal nerves and cell layers intact, allowing the wound to rapidly heal.
Following implantation through a 2-millimeter incision, the BPCDX successfully remained transparent. There was no scar formation or adverse reaction, and no intensive therapy or further surgery was required; just an eight-week treatment with immunosuppressive eye drops and a bandage.
The bioengineered cornea checked all the safety boxes.
After two years, the participants from Iran and India experienced an average increase of more than 200 micrometers in their cornea's thickness, and a decrease in its curvature, improving their vision at least to the extent of traditional corneal transplants.
Previously attempted biomaterial implants into the eye ended up thinning, but the fortified pig cell collagen held strong and kept the implant stable, even after eight years, the team reported based on their previous studies and unpublished data.
"No previous study has, to our knowledge, achieved full corneal transparency in vivo with sufficient corneal thickening and flattening, or with significant visual acuity gains as reported here," the researchers wrote in their paper.
A larger clinical trial is now being planned, but if the pilot is any indication the researchers are hopeful for additional promising results that will help the new procedure meet regulatory approvals.
"The results show that it is possible to develop a biomaterial that meets all the criteria for being used as human implants, which can be mass-produced and stored up to two years and thereby reach even more people with vision problems," Lagali concludes.
This research was published in Nature Biotechnology.
