A new study has uncovered a connection between malfunctions in the brain's waste removal processes, known as the glymphatic system, and an increased risk of psychosis – and it looks as though key changes could begin in early childhood.
The international team of researchers analyzed brain scan data from 85 individuals with 22q11.2 deletion syndrome (22q11DS), a genetic condition that comes with a significantly increased likelihood of developing psychotic disorders such as schizophrenia.
Because 22q11DS is linked to both a higher chance of psychosis and disruptions to different parts of the glymphatic system (such as the blood-brain barrier), the researchers wanted to study the condition to understand how broken waste removal mechanisms might trigger psychosis development.
The participants, part of a longitudinal cohort dedicated to studying those with 22q11DS and their healthy siblings, were scanned multiple times across 25 years.
Aged between 5 and 35 at the time of the scans, these scans gave the researchers a picture of how 22q11DS progresses from childhood into adulthood, and how associated changes compare with typical brain development.
Individuals with 22q11DS showed signs of impaired brain clearance early on, and among those who did go on to develop symptoms of psychosis, the glymphatic system didn't develop and expand as it normally would be expected to with age.
"This atypical trajectory suggests that a vulnerability resulting from an interaction between biological and environmental factors is present well before the onset of symptoms," says psychiatrist Alessandro Pascucci, from the University of Geneva in Switzerland.
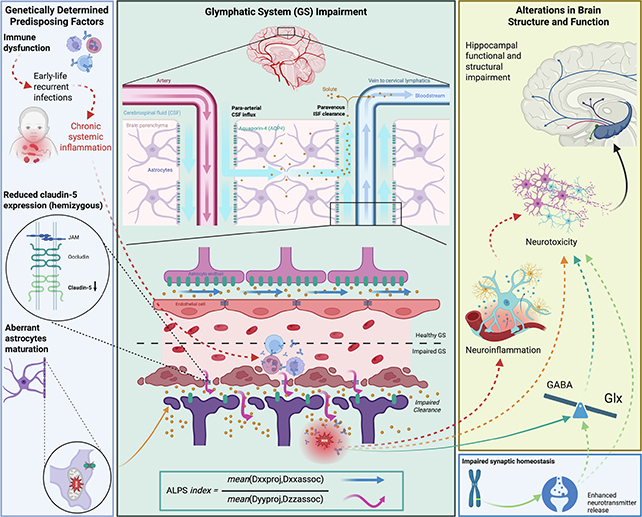
The researchers used a measure called the ALPS index to gauge glymphatic system function. Essentially, it measures water movement in the brain along crucial plumbing channels.
If those channels aren't flowing properly, it means all kinds of chemical waste and detritus are no longer being flushed from the brain. The waste that builds up can lead to inflammation and damage cells – and potentially, contribute to psychotic disorders.
As well as scoring ALPS, the researchers computed the balance between excitatory and inhibitory signals in the brain using data from a subset of 39 participants.
For optimal brain health, the neurotransmitters glutamate (which excites neurons) and gamma-aminobutyric acid (or GABA, which helps calm neurons) need to be carefully balanced. But in this study, those with less effective glymphatic systems – measured by lower water flow and lower ALPS scores – showed far more excitatory signals than calming ones.
"Excessive excitation can become toxic to neurons and contribute to alterations in certain brain regions that are particularly vulnerable and involved in psychosis, such as the hippocampus," says Pascucci.
The hippocampus is a part of the brain that's particularly vulnerable to stress and inflammation, and has previously been linked to psychosis.
"Our results suggest a link between glymphatic system dysfunction, mechanisms of neurotoxicity, and psychosis," Pascucci adds.
A malfunctioning glymphatic system is by no means exclusive to 22q11DS, but through this small group of participants, the researchers managed to gather some vital new clues about how poor 'brain cleaning' could be a factor in psychotic episodes and disorders.
If the warning signs hinted at here do indeed emerge early in life, it may mean there are opportunities to intervene before symptoms develop. Further studies of this critical window in development could also reveal more about how psychotic conditions develop in the first place.
Related: Annoying Cat Parasite Has Again Been Linked to Psychotic Episodes, But Only in Men
Most current psychotic treatments focus on trying to manage symptoms (such as hallucinations) after they've started appearing. With further research and development, we could now be on the way to finding treatments that take a more proactive and preventative approach.
"Identifying such modifiable predictive factors could pave the way for strategies to delay or even prevent a first psychotic episode," says psychiatrist Stephan Eliez, from the University of Geneva.
The research has been published in Biological Psychiatry: Global Open Science.

