Just like most parts of the human body, our eyes gradually deteriorate over time. A new study now shows how stress can accelerate this aging process, a discovery that could help us treat eye problems that develop as we get older, including the group of diseases responsible for vision loss known as glaucoma.
While the research is based on tests carried out on mice, the team thinks the same principles are likely to apply to human eyes as well.
A common consequence of psychological stress in even the healthiest of humans is a rise in intraocular pressure (IOP, aka ocular hypertension), or the fluid pressure in the eye. Known to be linked to the development of glaucoma, it seems the physiological stress of elevated IOP might also be linked to markers for biological aging, which can appear as changes in molecular tags on DNA and proteins that control which genes are switched on or off.
"The epigenetic changes we observed suggest that changes on the chromatin level are acquired in an accumulative way, following several instances of stress," says ophthalmologist Dorota Skowronska-Krawczyk, from the University of California, Irvine (UCI) School of Medicine.
"This provides us with a window of opportunity for the prevention of vision loss, if and when the disease is recognized early."
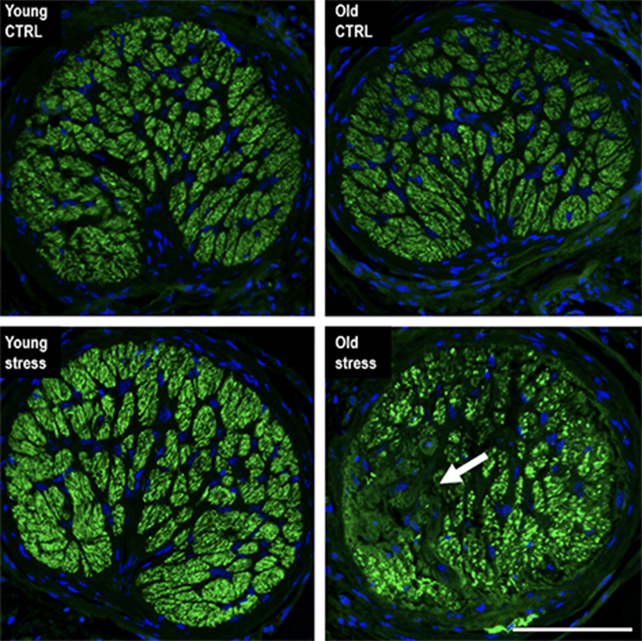
The team looked at the optic nerve head of mouse eyes – the place where retinal cells at the back of the eye converge to form the nerve that goes to the brain – in which IOP had been artificially elevated. In younger mice there was little difference when compared with control animals, but in older mice those with mildly elevated eye pressure showed a loss of axons or nerve fibers, which also happens with glaucoma cases.
To put it another way, the older mice seemed more susceptible to changes in pressure on their eyes, which leads to damage caused by inflammation and a gradual loss of cell function that would normally take years to develop naturally.
In humans, IOP isn't fixed, but oscillates through the day. More extreme and prolonged fluctuations have previously been associated with the progression of glaucoma, and the researchers behind the new study think that the cumulative effect of these fluctuations – and the pressure they put on the eye – is responsible for the aging of the tissue.
"Our work shows that even moderate hydrostatic IOP elevation results in retinal ganglion cell loss and corresponding visual defects when performed on aged animals," says Skowronska-Krawczyk.
"We are continuing to work to understand the mechanism of accumulative changes in aging in order to find potential targets for therapeutics. We are also testing different approaches to prevent the accelerated aging process resulting from stress."
Now that they have detected these pressure-induced changes, the researchers think they can use it as a way to assess the epigenetic age of tissue in the eye – the amount of wear and tear, essentially – and through that make treatments more targeted and more personalized for individual patients.
Psychological stresses aside, there are a number of other factors that can cause the pressure inside the eye to increase, from genetics to eye trauma to medications. However IOP increases, having a means of studying its impact could save the eyesight of millions.
As the worldwide population gets older, cases of glaucoma are expected to increase, and could reach as many as 110 million in 2040. If left untreated, these conditions can eventually lead to blindness.
While there's no way to reverse glaucoma damage completely, it can be managed – and being able to detect it (and the causes leading up to it earlier) would make a significant difference in eyesight loss.
"Our work emphasizes the importance of early diagnosis and prevention as well as age-specific management of age-related diseases, including glaucoma," says Skowronska-Krawczyk.
The research has been published in Aging Cell.