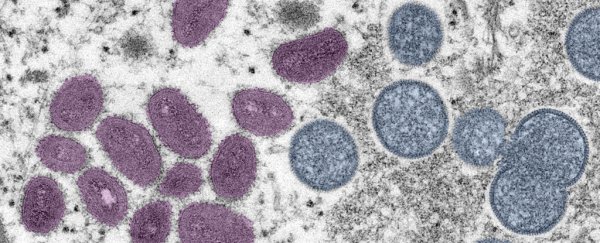
The monkeypox virus has mutated at a far faster rate than would normally be expected and likely underwent a period of "accelerated evolution," a new study suggests.
The virus, which has infected more than 3,500 people in 48 countries since its detection outside Africa in May, may be more infectious due to dozens of new mutations. In all, the virus carries 50 new mutations not seen in previous strains detected from 2018 to 2019, according to a new study published June 24 in the journal Nature Medicine.
Scientists usually don't expect viruses like monkeypox to gain more than one or two mutations each year, the study authors noted.
Monkeypox is a rare disease that virologists think may naturally circulate in monkeys and rodents. An orthopoxvirus, it comes from the same family and genus as the variola virus, which causes smallpox, and doesn't usually spread far beyond West and Central Africa, where it is endemic.
This year, however, the first widespread outbreak of the disease spread beyond Africa, surprising scientists and leading the World Health Organization (WHO) to begin considering whether to classify the outbreak as a global health emergency.
Monkeypox virus strains can be sorted into two clades, or lineages, known as the West African and Congo Basin clades, according to STAT. The viruses in each clade carry different fatality rates; the West African clade has a roughly 1 percent fatality rate, while the Congo Basin clade kills an estimated 10 percent of those it infects.
The ongoing outbreak appears to be driven by the West African clade, STAT reported.
Related: Monkeypox outbreaks: Here's everything you need to know
As a large double-stranded DNA virus, monkeypox is much more able to correct replication errors than an RNA virus such as HIV, meaning that the current monkeypox strain should have really only accumulated a handful of mutations since it first started circulating in 2018.
But, after collecting DNA from 15 monkeypox viral samples and reconstructing their genetic information, the researchers found that the real mutation rate was six to 12 times higher than they expected.
The massive jump in the monkey virus's rate of mutation "is far more than one would expect considering previous estimates of the substitution rate for Orthopoxviruses," the researchers wrote in the paper. "Our data reveals [sic] additional clues of ongoing viral evolution and potential human adaptation."
Historically, monkeypox is transmitted from person to person by close skin contact with open skin lesions, bodily fluids, contaminated material or respiratory droplets coughed into the air.
But the unprecedented speed of new infections could suggest that something may have changed about how the virus infects its hosts – and the new mutations could be a possible cause.
Many of the mutations identified by the researchers also carry telltale clues that they may have emerged due to the virus's contact with the human immune system, specifically a family of the virus-fighting enzymes called APOBEC3. These enzymes attack viruses by forcing them to make mistakes when they copy their genetic code, an act which usually causes the virus to break apart.
However, sometimes, the virus survives the encounter and simply picks up a few mutations in its genetic code, according to STAT. It may be that these sorts of battles happened repeatedly and caused the virus to pick up many mutations in a short span of time, the researchers theorized.
The virus's mutation rate ramped up in 2018, and there's a few explanations as to why it did so.
It's possible that the virus has been circulating in humans, at low levels, since then, picking up a slew of new mutations through its battles with enzymes.
Alternatively, the virus may have been spreading among animals in non-endemic countries without us noticing for quite some time, and then this year, it suddenly leapt back over to humans.
Or it's possible that, after a monkeypox outbreak hit Nigeria in 2017, the virus mostly spread in African countries – rapidly evolving as it moved between smaller communities before mounting a resurgence in non-endemic countries this year.
Despite its name, monkeypox is most commonly transmitted to humans from rodents, of which African rope squirrels, striped mice, giant-pouched rats, and brush-tailed porcupines are the species believed to be the main reservoirs of the disease, according to the Centers for Disease and Prevention.
The last time monkeypox was this widespread in the United States was in 2003, when 71 people became infected with the West African clade after a shipment of infected Gambian pouched rats, imported to Texas from Ghana, passed on the disease to local prairie dogs.
A direct treatment for monkeypox has yet to be tested, but doctors are administering antiviral drugs and antibodies taken from people immunized with the smallpox vaccine to patients.
Transmission is also reduced if people have the monkeypox or smallpox vaccine, enabling scientists to prevent onward infections by inoculating the close contacts of an initial case – a strategy known as "ring vaccination" that led to the eradication of smallpox in 1980.
Related content:
Going Viral: 6 New Findings about Viruses
The deadliest viruses in history
Do other viruses have as many variants as SARS-CoV-2?
This article was originally published by Live Science. Read the original article here.