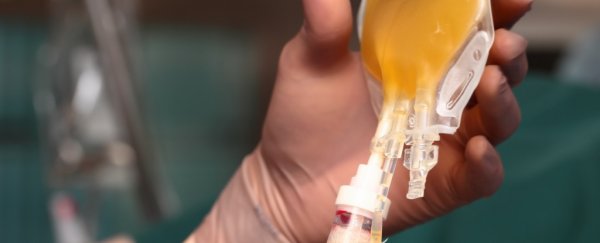
During the 1918 Spanish flu pandemic, doctors discovered they could treat sick patients with the blood of those who had already recovered. The therapy, known as convalescent plasma, helped reduce mortality among people with acute infections.
Now, the FDA has issued an emergency authorization for the therapy's use among COVID-19 patients.
Antibodies develop in plasma, the liquid portion of blood – they're part of our body's natural response to a foreign pathogen. So the idea behind the treatment is to help sick people mount an antibody response to the virus by transferring plasma intravenously from those who already have antibodies.
"What we really need are drugs that, when given early, can prevent a symptomatic person from requiring hospitalisation or very dramatically diminish the time that they're symptomatic," Dr Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, told Facebook founder Mark Zuckerberg last month.
Convalescent plasma is especially promising in that regard.
The emergency use authorization from the FDA will allow doctors to administer the treatment earlier in the course of an infection, when it's believed to be most effective. The agency was expected to authorize plasma treatment last week, but it was briefly delayed after federal health officials, including Fauci, called for more data from randomised control trials, The New York Times reported.
Dr Thomas File, president of the Infectious Diseases Society of America, said the available data on the treatment is still insufficient.
"While the data to date show some positive signals that convalescent plasma can be helpful in treating individuals with COVID-19, especially if given early in the trajectory of disease, we lack the randomised controlled trial data we need to better understand its utility in COVID-19 treatment," he said in a statement on Sunday.
As of Monday, more than 2,700 hospitals have already administered plasma therapy through an expanded-access program led by the Mayo Clinic. The program has delivered plasma to more than 100,000 patients, according to the program website.
However, there are still major limitations to plasma therapy's widespread use. Plasma must be transferred quickly from a donor to a recipient – and both must have compatible blood types. The quantity is also limited, since it depends on blood donations.
That means plasma isn't likely to be a long-term treatment for the virus. Instead, researchers and pharmaceutical companies see it as an interim therapy until a vaccine becomes readily available.
Early research shows promise
A national study of 35,000 hospitalized coronavirus patients, which is still awaiting peer review, found that patients less than 80 years old who weren't on a respirator and received plasma containing high levels of antibodies within three days of their diagnosis had a 35 percent lower mortality rate than those who were treated four or more days after their diagnosis.
In a White House briefing on Sunday, Health and Human Services Secretary Alex Azar called this "a major advance in the treatment of patients."
But researchers would ideally need to compare patients who received plasma with untreated patients to know whether the therapy really impacts survival.
A May study from researchers at Mount Sinai – which is still awaiting peer review – found that hospitalized coronavirus patients who received convalescent plasma had a higher chance of survival than those who didn't receive the treatment: Only 18 percent of the plasma recipients saw their conditions worsen two weeks after their transfusion compared to 24 percent of patients who didn't receive the treatment.
By May 1, nearly 72 percent of the plasma recipients had been discharged from the hospital compared to 67 percent of the other patients. But the study was small – only 39 patients received transfusions – and the results were only significant for patients who didn't need a ventilator.
In another study (also not yet peer reviewed), researchers at the Mayo Clinic found that convalescent plasma reduced the mortality rate among hospitalized coronavirus patients by 57 percent.
Most research so far has suggested that patients treated earlier in the course of their infection have better outcomes.
A recent study of 316 patients at Houston Methodist hospitals found that patients who received plasma transfusions within 72 hours of being admitted to the hospital had a lower risk of mortality over the next 28 days than patients who received transfusions after 72 hours had passed.
"We now have more evidence than ever that this century-old plasma therapy has merit, is safe, and can help reduce the death rate from this virus," Dr James Musser, chair of the Department of Pathology and Genomic Medicine at Houston Methodist, said in a statement.
Mayo Clinic researchers also determined that the treatment was relatively safe among 5,000 adults with severe or life-threatening cases. Less than 1 percent of the patients developed severe side effects within four hours of receiving a blood transfusion. Although transfusions always pose some risk to seriously ill patients, only four deaths were linked to the plasma therapy.
Drug companies are converting plasma into medicine
In May, a coalition of medical institutions, drug companies, nonprofits, and COVID-19 survivors launched "The Fight Is In Us" – a campaign to get more recovered coronavirus patients to donate blood. Some of that blood will be used for direct transfusions, and the rest will go toward manufacturing hyperimmune globulin, a drug built from convalescent plasma.
The process of creating hyperimmune globulin involves pooling plasma from recovered patients and heat-treating it so that any remaining pathogens get destroyed. The result is a vial of medicine with consistent antibody levels that can easily be administered to patients. The drug focuses on the most common antibody found in blood – immunoglobulin G (IgG) – which usually confers long-term immunity.
"It's basically treated in a way that reduces the likelihood that it could pass on any infections," David Reich, president and chief operating officer of The Mount Sinai Hospital, told Business Insider in April. "Something like that could be helpful, potentially, to people in the early phase of the disease or potentially as prophylaxis against the disease."
Mount Sinai is working with Emergent BioSolutions, a Maryland-based biopharmaceutical company, to develop a hyperimmune globulin product. The group will study whether the drug can protect individuals at high risk of exposure, such as healthcare workers, from getting infected in the first place.
A coalition of 10 drug companies involved in the "The Fight Is In Us" campaign is also creating a hyperimmune globulin drug. The research is led by Takeda, Japan's largest pharmaceutical company, and CSL Behring, a Pennsylvania-based biotech company. They're hoping to determine whether hyperimmune globulin improves outcomes for coronavirus patients with severe cases.
"Our goal here isn't to continue to produce hyperimmune globulin ad infinitum," Christopher Morabito, head of research and development for plasma-based therapies at Takeda, previously told Business Insider. "Our goal here is to have an effective therapy to bridge us to a point where either the pandemic is over because it dies out, or because there's a vaccine available, or until there are many more effective treatments for patients with this disease."
The coalition hopes to secure regulatory approval from the FDA by the end of 2020. But there are plenty of hurdles: Drug quantities are still limited by the quantity of plasma people donate.
Companies researching hyperimmune globulin and direct convalescent plasma treatments also still need to prove that the approaches are safe.
This story has been updated with new information. It was originally published August 11, 2020.
This article was originally published by Business Insider.
More from Business Insider: