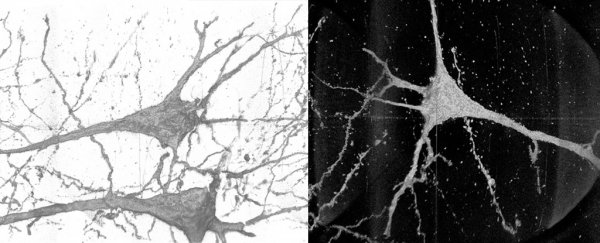
Capturing details of brain cells on a nanometre scale, researchers have uncovered evidence that the neurons of people with schizophrenia could have unique differences in thickness and curvature, and this might even account for some of their symptoms.
The finding comes from an analysis on just a small handful of donors, and is a long way from demonstrating how contrasting nerve cell structures might explain the neurological condition.
But as our understanding of these unusual characteristics grows, it could lead to better methods of treatment, helping give tens of millions around the world a better quality of life.
The study, led by researchers from Tokai University in Japan, made use of two different X-ray microscope technologies, one at the SPring-8 light source facility in Japan, the other at the US Department of Energy's Advanced Photon Source (APS).
Both of these accelerate particles along curving paths in what's known as a synchrotron, causing them to shed short wavelengths of electromagnetic radiation in the X-ray part of the spectrum.
Using X-rays as a radiation source for photographing fine details of tiny objects - such as neurons - can be a bit of a double-edged sword.
On one hand, their tight wavelengths are just the thing to capture every buckle and weave of a cell's membrane. The APS is capable of a resolution down as far as 10 nanometres, a scale that brings it remarkably close to revealing the texture of individual protein channels peppering a cell membrane.
Viewed from enough angles, it's possible to reconstruct neurons as high definition, three-dimensional terrains.
Unfortunately, as tiny as neurons are, they're also quite long. Tracing every bump of their surface is tedious work when you need to creep your way along entire millimetres of their body.
"The sample has to move through the X-ray beam to trace the neurons through the sample," says Vincent De Andrade, a physicist in Argonne's X-ray Science Division.
"The field of view of our X-ray microscope is about 50 microns, about the width of a human hair, and you need to follow these neurons over several millimetres."
Taking samples of tissue from a select part of the brain in four deceased individuals diagnosed with schizophrenia, and four without, the team undertook the tedious work of scanning nerve cells using the two different synchrotron facilities.
The images were combined to reconstruct the neurons as digital models, which contributed to a larger dataset that could be statistically compared and contrasted in search of distinguishing characteristics.
They found, statistically speaking, the thickness and curvature of cellular features extending away from the neuron's body was significantly different among individuals with schizophrenia, compared to those without the condition.
These variations could affect how the neurons transmit messages down their lengths, which might go some way to explain characteristics of the disorder, which in its most serious forms includes hallucinations, impeded motor control, and delusions.
Exactly what is behind such deviations in cellular geometry, or whether the variations extend all the way to the synaptic 'toes' of the neuron, will require even more detail than current generation synchrotrons can manage.
That could change when the APS gets a US$815 million upgrade in the next few years that will see it produce far X-ray beams 500 times brighter than those it currently emits.
"The APS upgrade will allow for better sensitivity and resolution for imaging, making the process of mapping neurons in the brain faster and more precise," says De Andrade.
"We would need resolutions of better than 10 nanometres to capture synaptic connections, which is the holy grail for a comprehensive mapping of neurons, and those should be achievable with the upgrade."
Piecing together the mechanisms behind schizophrenia's development is a complex process that will require advanced imaging and computational technology.
We're gradually coming to understand the multitude of genetic and environmental factors that see the brain change while still in the womb, and continue to shift as a child grows into adulthood.
If there are ways this can be spotted and treated early, we could help limit, if not prevent the worst of the traits that can put people at risk of a serious mental illness.
This research was published in Translational Psychiatry.