Certain genetic variants, carried by around 10 percent of the population, could be making type 2 diabetes GLP-1 treatments (such as Ozempic and Wegovy) less effective, according to new research.
These treatments are named after the glucagon-like peptide-1 (GLP-1) hormone that they simulate. In the case of diabetes, that means regulating blood sugar by boosting insulin and slowing down digestion.
However, the impact of GLP-1 drugs on people with type 2 diabetes can vary considerably. The international team of researchers behind the new study wanted to see whether genetics may be playing a part.
To investigate, the team focused on an enzyme called PAM (short for peptidyl-glycine alpha-amidating monooxygenase), and the gene that encodes it.
Around 1 in 10 people carry variants in the PAM gene that can interfere with the activation of hormones, including GLP-1. PAM variants are also more common in people with diabetes.
"When I treat patients in the diabetes clinic, I see a huge variation in response to these GLP-1-based medications and it is difficult to predict this response clinically," says endocrinologist Mahesh Umapathysivam, from Adelaide University in Australia.
"This is the first step in being able to use someone's genetic makeup to help us improve that decision-making process."
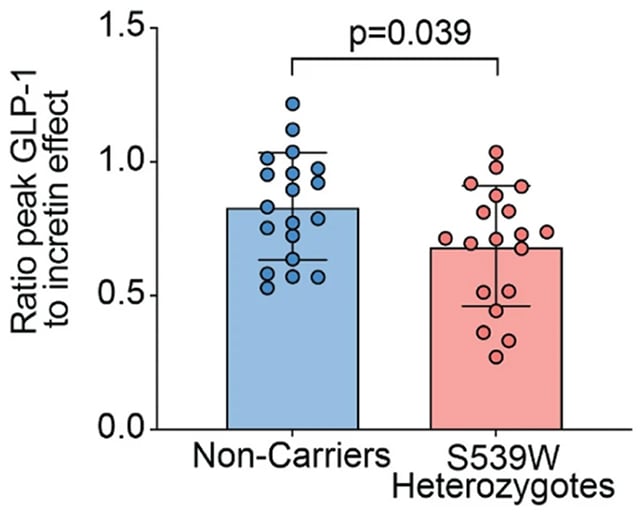
In their analysis, the researchers compared 19 people with the PAM gene variant p.S539W to 19 matched controls, studying how their bodies tolerated consuming a sugary drink.
Surprisingly, those with the variant showed an abundance of GLP-1 in their system. It turned out p.S539W was creating GLP-1 resistance, stopping the hormone from being properly processed by the body.
"Despite people with the PAM variant having higher circulating levels of GLP-1, we saw no evidence of higher biological activity," says endocrinologist Anna Gloyn, from Stanford University.
"They were not reducing their blood sugar levels more quickly. More GLP-1 was needed to have the same biological effect, meaning they were resistant to GLP-1."
This switch around was so unexpected, the researchers ran further tests on mouse models with the PAM gene deactivated. This meant no PAM enzyme, and the mice developed signs of GLP-1 resistance too, with blood sugar left unregulated despite elevated levels of GLP-1.
The team didn't stop there, either. The next step was to analyze clinical trials covering a total of 1,119 participants, to see if people with specific PAM variations were reacting less favorably to GLP-1 drugs.
Again, the findings backed up the idea that these genetic variants lead to GLP-1 resistance: Those who had the standard PAM gene variants reacted better to GLP-1 medication than those who didn't. This connection wasn't seen with the other diabetes drugs trialed.
There's plenty of scope for future research here. The exact mechanisms that are preventing GLP-1 drugs from having an effect still need to be investigated.
Researchers could also look at the relationship between PAM genes and GLP-1 drugs prescribed for weight loss, which typically means a higher dosage.
Potentially, genetic tests could now help determine whether or not GLP-1 treatments will work for individuals with type 2 diabetes – meaning less time and money is wasted on drugs that aren't going to be effective.
There might also be opportunities for GLP-1 drugs to be modified somehow to circumvent the impacts of these PAM gene variations – but it's still early days in that regard.
Related: Stopping GLP-1 Drugs Triggers Weight Regain 4x Faster Than Ending Exercise
"It's very common for pharmaceutical companies to collect genetic data on their participants," says Gloyn.
"For the newer GLP-1 medications, it would be useful to look at whether there are genetic variants, like the variants in PAM, that explain poor responders to their medications."
"There are a whole class of medications that are insulin sensitizers, so perhaps we can develop medications that will allow people to be sensitized to GLP-1s or find formulations of GLP-1, like the longer-acting versions, that avoid the GLP-1 resistance."
The research has been published in Genome Medicine.

