Valproic acid – a drug commonly used to treat epilepsy and bipolar disorder – can cause birth defects and developmental disorders if taken during pregnancy, but the reason why has long been a mystery.
Now, in a study using mice and human tissue, scientists discovered that the medication locks some embryonic cells into a suspended state where they can't properly grow or divide.
By forcing key stem cells cells into this state, called senescence, valproic acid may disrupt brain development in the womb and therefore cause cognitive and developmental disorders down the line, according to the study, published Tuesday (June 14) in the journal PLOS Biology.
An estimated 30 to 40 percent of infants exposed to the drug in the womb develop cognitive impairments or autism spectrum disorder, the study authors noted in their report, and these laboratory studies hint at why that happens.
In a subset of affected children, valproic acid exposure can also cause birth defects beyond the brain, including heart malformations and spina bifida, where part of the spinal column doesn't form properly and thus leaves the spinal cord exposed.
However, the new study suggests that these physical birth defects, though also linked to valproic acid, are triggered by a different mechanism than the cognitive impairments, Bill Keyes, a team leader at the Institute of Genetics, Molecular and Cellular Biology in Strasbourg, France and senior author of the study, told Live Science.
Related: Brain differences tied to autism can be detected in the womb
Mice and mini-brains
When taken as a treatment for epilepsy or bipolar disorder, valproic acid affects the body in several ways, according to the online medical database StatPearls. For instance, the medication changes the levels of certain chemical messengers in the brain and alters which genes can be switched on in a cell at any given time.
Valproic acid first hit the market in the 1960s as an anticonvulsant medication, but by the 1980s, the drug's link to birth defects became apparent, according to BBC News.
Later research in rodents and monkeys suggested that, when taken in the first few weeks of pregnancy, the drug might disrupt the earliest stages of nervous system formation.
This upset seems to occur around the time that the "neural tube" – a hollow tube of tissue that later becomes the brain and spinal cord – forms and closes. In human embryos, that's typically between the fourth and sixth week of pregnancy, according to the Centers for Disease Control and Prevention (CDC).
To understand how valproic acid messes with this early stage of development, Keyes and his colleagues exposed mouse embryos to the drug. The neural tubes of these exposed embryos often failed to close, and later in development, the fetal mice also grew unusually small heads and brains.
Rodent cells exposed to valproic acid carried enzymes that only appear in cells undergoing senescence; the same enzymes did not crop up in the cells of healthy, unexposed mice. These markers of senescence specifically appeared in exposed neuroepithelial cells, a type of stem cell that later produces brain cells.
To check if valproic acid could trigger senescence in human cells, the team ran a similar experiment using 3D clusters of human nerve cells, known as cerebral organoids.
These organoids resemble miniature human brains, in that their structure and function is similar to that of the full-size organ. The researchers exposed the organoids to valproic acid and found that the drug pushed the organoids' neuroepithelial cells into senescence, just as it had in the mouse embryos.
Related: Father's use of diabetes drug could raise his kids' risk of birth defects
"This was just very nice validation for us to be able to set up and test organoids and then see that we were seeing senescence in exactly the same cell type," Keyes said. And because the valproic acid exposure nudged the organoids' neuroepithelial cells into a suspended state, the exposed organoids turned out much smaller than organoids that hadn't been exposed to the drug.
How exactly does valproic acid push cells into senescence? It yanks the brakes off a specific gene that usually stays inactive throughout embryonic development, the team discovered.
This gene codes for a molecule called p19Arf, which usually becomes active in adulthood and helps to clear cancerous and aging cells from the body. Although helpful in adults, the molecule's presence in embryos drives key cells into senescence and disrupts the development of the nervous system.
When the team genetically modified mice so that they couldn't produce p19Arf, the rodents became impervious to some of valproic acid's effects, and the mice's brains were able to grow to normal size.
However, the mice still developed deformities in their spinal cords, which suggests that valproic acid causes those defects through a different mechanism, Keyes said.
"I think it is a strength of the study to utilize both human organoids and mouse model systems," said Richard H. Finnell, a professor in the Center for Precision Environmental Health and various other departments at Baylor College of Medicine, who was not involved in the research.
The organoid experiments confirmed which genes are affected by valproic acid exposure, and the mouse model revealed how the drug's effects unfold in ongoing pregnancies, he told Live Science in an email.
Nevertheless, "there are many caveats to our model", Keyes said.
For instance, the team exposed their mice and organoids to several high doses of valproic acid over a short period of time, whereas in real life, patients consistently take a lower dose of the drug over a longer time span.
The high-dose, short-term regimen in the experiments may therefore have triggered an "exaggerated" effect in the mice and organoid cells that wouldn't necessarily be matched in human embryos, Keyes said.
In other words: Although the mice and organoids in the study showed senescence in a large portion of their neuroepithelial cells, the effect on human embryos would likely be patchier, he said.
"So then the child would ultimately be born with some defects in some population of cells," he said, and in theory, "this then gives rise to the cognitive and behavioral defects."
In the future, the team hopes to repeat their lab experiments with a valproic acid regimen that more accurately mirrors real-world exposure, meaning one that's low-dose and long-term, Keyes said.
These experiments, along with in-depth genetic analyses, should reveal more details of how valproic acid exposure impacts growing human embryos.
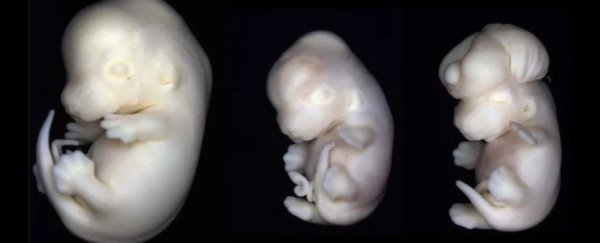
Caption for top image: Mouse embryos exposed to valproic acid in the womb develop similar birth defects to human embryos. The far left mouse embryo in this photo was not exposed to the drug, but the right two were. The center embryo has microcephaly (a small head) and the one on the far right has exencephaly (where part of the brain is exposed).
Related content:
This brain structure may grow too fast in babies who develop autism
This article was originally published by Live Science. Read the original article here.