Should members of the public be wearing face masks during the COVID-19 pandemic? It's a controversial question, with different countries and authorities giving different advice.
We have reviewed the results of more than a dozen randomised trials of face masks and transmission of respiratory illnesses. We found the current best evidence suggests wearing a mask to avoid viral respiratory infections such as COVID-19 offers minimal protection, if any.
Conflicting recommendations
Two of the world's major health organisations disagree on mask wearing. The World Health Organisation (WHO) currently discourages mask use:
There is currently no evidence that wearing a mask (whether medical or other types) by healthy persons in the wider community setting, including universal community masking, can prevent them from infection with respiratory viruses, including COVID-19.
WHO does recommend special masks (N95 masks or equivalent) plus other protection for health-care workers working with people who have, or are suspected to have, COVID-19.
By contrast, the Centres for Disease Control and Prevention (CDC) in the United States has recently recommended everyone wear a (cloth) mask. However, this is to prevent infected people passing on the infection, not to prevent the wearer getting infected.
Who is right? Does wearing a mask protect the wearer? Does it protect others?
Understanding the spread
To examine this, we need to first look at how coronavirus spreads and how masks might stop it.
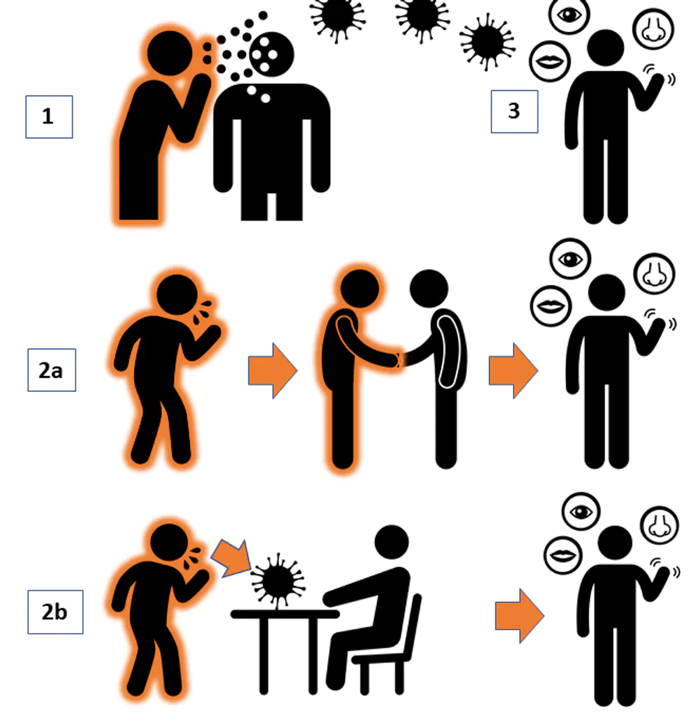 How coronavirus can be transmitted directly. (Author provided)
How coronavirus can be transmitted directly. (Author provided)
There are several possible routes to infection. An infected person can cough, sneeze or breathe while within about two metres of another person, and the virus lands in the other person's eyes, nose or mouth (1).
Another route is when an infected person coughs or sneezes onto their hand or onto a surface. The uninfected person then shakes the hand (2a) or touches the surface (2b), and transfers the virus to their own eye, nose or mouth.
It is possible that an infected person can also cough or sneeze to create an airborne spread (3) beyond the close contact range – but it is controversial whether this last route is a major means of transmission.
We don't know how much transmission occurs by each of these routes for COVID-19. It's also unclear how much protection a mask would offer in each case.
Current best evidence
To resolve this question, we analysed 14 randomised trials of mask wearing and infection for influenza-like illnesses. (There are no randomised trials involving COVID-19 itself, so the best we can do is look at similar diseases.)
When we combined the results of these trials that studied the effect of masks versus no masks in health-care workers and the general population, they did not show that wearing masks leads to any substantial reduction of influenza-like illness. However, the studies were too small to rule out a minor effect for masks.
Why don't masks protect the wearer?
There are several possible reasons why masks don't offer significant protection. First, masks may not do much without eye protection. We know from animal and laboratory experiments that influenza or other coronaviruses can enter the eyes and travel to the nose and into the respiratory system.
While standard and special masks provide incomplete protection, special masks combined with goggles appear to provide complete protection in laboratory experiments. However, there are no studies in real-world situations measuring the results of combined mask and eyewear.
The apparent minimal impact of wearing masks might also be because people didn't use them properly. For example, one study found less than half of the participants wore them "most of the time". People may also wear masks inappropriately, or touch a contaminated part of the mask when removing it and transfer the virus to their hand, then their eyes and thus to the nose.
Masks may also provide a false sense of security, meaning wearers might do riskier things such as going into crowded spaces and places.
Do masks protect others?
Could masks protect others from the virus that might have been spread by the mask wearer? A recent Hong Kong laboratory study found some evidence masks may prevent the spread of viruses from the wearer.
They took people with influenza-like symptoms, gave half of them masks and half no masks, and for 30 minutes collected viruses from the air they breathed out, including coughs.
Masks did reduce the amounts of droplets and aerosols containing detectable amounts of virus. But only 17 of the 111 subjects had a coronavirus, and these were not the SARS-CoV-2 coronavirus. While the study is promising, it needs to be repeated urgently.
We also don't know how this reduction of aerosols and droplets translates to reduction of infections in the real world. If there is an effect, it may be diluted by several factors such as ill people who don't wear a mask and "well" people who have no symptoms but are still carrying and spreading the virus.
Masks for some?
If wearing masks does substantially reduce the spread of the infection to others, what should we do? We could ask everyone with any respiratory symptoms to wear masks in public. That could supplement other strategies such as social distancing, testing, tracking and tracing to reduce transmission.
To also capture infected people without symptoms, we could ask everyone to wear masks in indoor public spaces. Outdoors is more difficult, since most people pose little or no risk. Perhaps, as we reduce restrictions, masks could also be required at some outdoor crowd events, such as sporting events or concerts.
Another possibility is a "2 x 2" rule: if you are outdoors and within 2 metres of other people for more than 2 minutes you need to wear a mask.
Mask wearing for the possibly infected, to prevent spreading the infection, warrants rigorous and rapid investigation. It could be an alternative or a supplement to social distancing, hand hygiene, testing, and lockdowns.
The authors would like to thank John Conly, Liz Dooley, Lubna Al-Ansary, Susan Michie and Amanda McCullough for comments.![]()
Paul Glasziou, Professor of Medicine, Bond University and Chris Del Mar, Professor of Public Health, Bond University
This article is republished from The Conversation under a Creative Commons license. Read the original article.
