An undesigned 'natural' experiment in one of the United States' most polluted cities has shown us the real-world benefits of cleaning up and shutting down coal-fired power plants.
The quality of air we breathe is well known to have a constant impact on human health. So it makes sense that coal plants belching dangerous particulate matter above our heads aren't exactly good for us.
The state of Kentucky has long ranked among the top five US states for sulfur dioxide and nitrogen dioxide emissions, both of which can come from coal plants and cause human health issues.
In the past, numerous studies have shown that people who live near these facilities have more asthmatic symptoms and other respiratory health problems. Yet so far, it's been difficult to tie these maladies directly to burning coal.
A unique quasi-experiment in the city of Louisville has now allowed us to bridge that gap like never before.
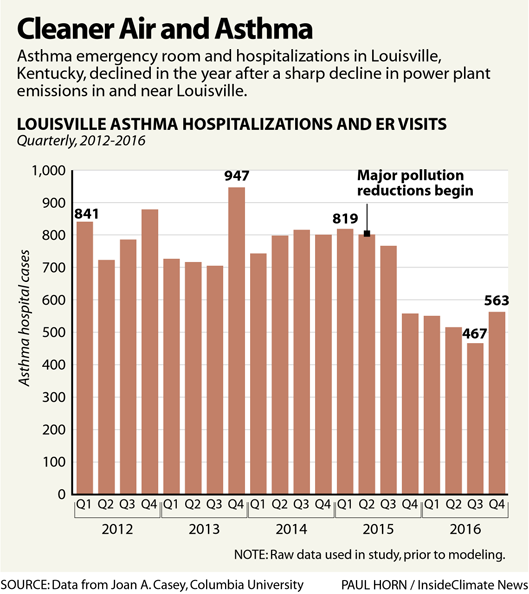
Between 2013 and 2016, one coal plant was retired near Louisville and another three installed stricter emission controls, adding SO2 scrubbers to their stacks (which dramatically cut SO2 emissions) and causing abrupt changes in the air quality of the region.
The situation was too perfect, and researchers jumped at the opportunity to frame a natural experiment.
The team used long-term emission models and digital sensors on asthmatic inhalers to explore asthma-related hospitalisations at a zip code level and also respiratory issues at an individual level.
"We saw about three fewer emergency department visits and hospitalisations per quarter per zip code," Joan Casey, an environmental health scientist from Columbia University, told Environmental Health News.
"That translates into about 400 prevented asthma-related hospital visits per year across the county."
What's more, that significant number came after the researchers accounted for other potential changes in air quality unrelated to power plants, such as vehicle emissions.
According to the authors, this real-life experiment is better than other observational studies because it can sort of mimic pseudo-randomisation of individuals and populations at differing levels of air pollution, which makes it easier to infer causal relationships.
In Beijing, for instance, when officials were determined to clean up the air quality for the Olympics, scientists were able to use a similarly quasi-experimental design to show changes in asthma-related hospitalisations and emergency department visits.
The new study, however, goes a step further. It measures asthma morbidity based on hospitalisation and daily symptoms.
After changes had been made to the four local Louisville coal plants in 2015, researchers calculated a 55 percent reduction in the amount of lung-irritating pollutants in the city's air.
This abrupt change was then tied to substantially fewer asthma-related problems in the hospital and the home.
The latter aspect was achieved using a project called AIR Louisville, which uses digital inhaler sensors to gain insights into the impact of local air quality among 1,200 members of the community.
Tapping into these data in the month after scrubbers were installed at a coal plant in Mill Creek, researchers saw a 17 percent drop in the use of inhalers among 207 local asthma patients.
"This is the first study to use digital inhaler sensors to understand the health effects of reducing emissions from coal-fired power plants," says population health researcher Meredith Barrett, who works for the company that distributed the digital inhalers.
"We hope this evidence will encourage government officials to support stricter standards when regulating coal-fired power plants and encourage us towards cleaner power options, thereby protecting the health of the people who live near these facilities."
At the time the data were collected, all four coal plants contributed the bulk of sulphur dioxide pollution in Louisville, and this pollution was found in every single zip code.
In a city of over 600,000 people, that's an astonishing number of residents who were breathing pollutants every single day.
In a contribution to Nature Energy, Casey argues the timing of these results is important. The US EPA is currently suspending enforcement of environmental laws during the COVID-19 pandemic.
"The US has stark environmental inequities, with poorer communities and communities of colour facing a disproportionate burden of air pollution as well as elevated rates of asthma and other respiratory diseases," she notes.
"Members of these communities appear at greatest risk of COVID-19 infection and death. In a time of need the US EPA has stopped protecting those who need it most."
The study was published in Nature Energy.
