It's been known for some time that psychological stress can make eczema (atopic dermatitis) worse, but it hasn't been clear how or why. Now, a new study may have uncovered the specific nerve pathway responsible for the link.
Using mouse models of eczema, researchers discovered a connection between the nervous system and the immune system centered around a specific group of 'fight-or-flight' nerves plugged into the skin. Under stress, these nerves activate white blood cells called eosinophils, which, in their efforts to protect the body from potential invaders, can end up irritating the skin.
The researchers, led by a team from Fudan University in China, believe their findings could improve eczema treatments, as their results suggest that managing psychological stress might be one way to lessen the severity of the skin disease.
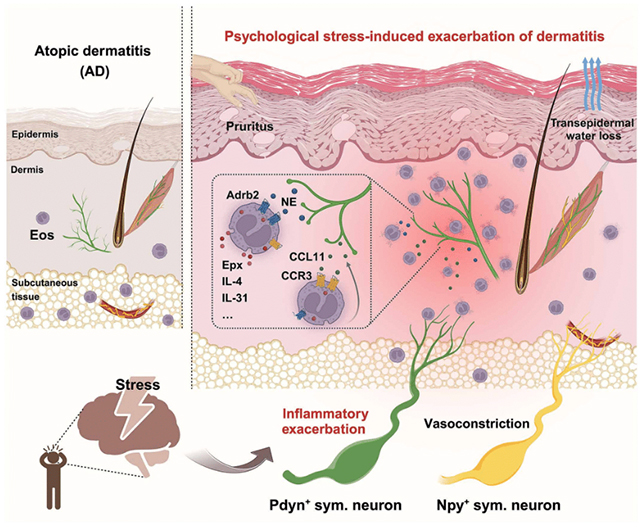
The research started with a group of 51 people with eczema. The study team compared their self-reported stress levels with the severity of inflammation on their skin and the levels of eosinophils within it.
There was a direct link between stress levels and eczema severity, the researchers found. Internally, though, this was mainly shown through higher levels of eosinophils in the blood and skin, rather than changes in other types of immune cells.
That led to further investigations using mouse models of eczema. By putting the animals into high stress situations and using a combination of advanced imaging and genetic analysis techniques, the team traced the link between stress and eczema – mapping the precise wiring between the brain's stress-reporting regions and the skin.
This led to the chain reaction that starts with 'fight-or-flight' nerves (known as sympathetic neurons) and ends with a worsening skin rash, driven by eosinophils being pushed into an unusually damaging mode.
When the mice were genetically engineered to have fewer eosinophils, the association between extra stress and a worsening skin rash largely went away, though the eczema itself remained. That's something that could be looked at in future studies.
"These findings deepen our understanding of the distinct properties of sympathetic neurons in skin inflammation… with potential implications for developing targeted strategies to block specific neuronal subtypes in skin diseases," write the researchers.
It's not the first time eosinophils have been identified as drivers of eczema irritation, but previous studies have been inconclusive about how effective treatments targeting these immune cells could be.
The new discoveries suggest that eosinophils are influencing the way stress exacerbates eczema, though perhaps not driving the condition itself.
Related: Each Stressful Person in Your Life May Age You by Months, Study Finds
Up to 10 percent of the adult population is known to get eczema, and atopic dermatitis (the type studied here) is the most common form. It can cause skin pain, severe itchiness, and disrupted sleep patterns – so anything that could be done to alleviate those symptoms would be welcome.
In a linked commentary on the study, immunologists Nicolas Gaudenzio and Lilian Basso from the University of Toulouse in France suggest that the brain might be holding on to a 'memory' of past eczema inflammation, which gets triggered again under stress.
All of these ideas can be examined in further studies, and several key questions remain, including how this newly identified stress pathway might be involved in other inflammatory conditions.
"It is unclear how different types of psychological stress (acute or chronic, physical or emotional) engage the neuroimmune axis that the authors identified," Gaudenzio and Basso write in their commentary.
"Whether other immune cell types or neuronal subtypes are involved in this process is also unknown. Research into the existence of similar mechanisms in other stress-sensitive inflammatory diseases, such as psoriasis or inflammatory bowel disease, is also needed."
The research has been published in Science.