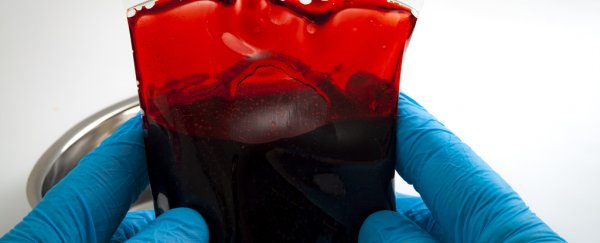
Blood from recovered coronavirus patients could be used in a vital stop-gap treatment to help protect humanity from the COVID–19 pandemic currently spreading around the world, researchers propose.
In a new paper, infectious disease experts explain how viral antibodies, contained in the blood serum of patients who have already recovered from the new coronavirus, could then be injected into other people, offering them short-term protection.
This long-established medical remedy – called passive antibody therapy – dates back to the late 19th century, and was widely used during the 20th century to help stem outbreaks of measles, polio, mumps, and influenza.
Much as it aided us before, it could be a crucial and practical tool now in the fight against COVID–19, a team from Johns Hopkins University argues in the new study, adding that antibody therapies can also be made available with urgency.
"Deployment of this option requires no research or development," says immunologist Arturo Casadevall.
"It could be deployed within a couple of weeks since it relies on standard blood-banking practices."
For the treatment to work, recovered coronavirus patients would need to donate their blood after recovering from COVID–19 and while still convalescing from the disease. During this phase, the blood serum would contain high amounts of natural antibodies produced to combat the SARS-CoV–2 virus.
Once the body produces them in response to pathogens, such antibodies can remain circulating in the blood for months and even years after an infection.
But these antibodies aren't just useful for the recovered individual. If we extract and process them, antibodies can be injected into other people to provide a short-term benefit; this could be used for patients at serious risk, uninfected family members of an infected patient, or to bolster the immunity of medical workers at greater exposure to the pathogen.
"Passive antibody administration is the only means of providing immediate immunity to susceptible persons," the researchers explain in their paper.
"Depending on the antibody amount and composition, the protection conferred by the transferred immunoglobulin can last from weeks to months."
Using modern blood banking techniques – which can screen for other kinds of infectious agents that might be contained in blood – the therapy is arguably low risk for healthy people, the researchers say, especially in comparison to the threats inherent in the COVID–19 outbreak, for which there are no vaccines or drugs currently available.
Against that backdrop, the team proposes that the use of convalescent sera should be considered as an emergency response to help protect against COVID–19, just as it was trialled against other coronavirus diseases of this century, including SARS1 and MERS.
Of course, COVID–19, being a pandemic, is on a much larger scale to those smaller outbreaks – but that sad reality will actually help the making of convalescent sera supplies, as there will be a much greater number of recovered coronavirus patients who could supply their blood.
At time of writing, over 77,000 people have already recovered from COVID–19, according to John Hopkins University's latest statistics on the outbreak (which are updated frequently); their blood could readily help make vital antibodies for others, whereas other sorts of antiviral treatments and a much-hoped-for vaccine are expected to take considerably longer to develop.
"In addition to public health containment and mitigation protocols, this may be our only near-term option for treating and preventing COVID–19, and it is something we can start putting into place in the next few weeks and months," Casadevall says.
To that end, John Hopkins University is funding efforts to begin setting up antibody therapy operations for COVID–19 in the Baltimore area in the coming weeks. Doctors in New York are also investigating the treatment, Casadevall says, while internationally, Japan's largest pharmaceutical company is looking at developing an antibody-based drug to combat coronavirus.
There are still a lot of unknowns, including how much convalescent serum is needed to be effective to protect people, but early, unconfirmed media reports from China suggest this therapy is already working there.
Nobody is expecting passive antibody therapy to become a silver bullet for the new coronavirus, but as something that could help us flatten the curve while other treatments are developed, it could make a huge difference, if we all act together – and act quickly.
"Clearly, the use of convalescent serum would be a stopgap measure that could be used in the midst of the current epidemic," the authors write.
"However, even local deployment will entail considerable coordination between different entities… Hence, as we are in the midst of a worldwide pandemic, we recommend that institutions consider the emergency use of convalescent sera and begin preparations as soon as possible. Time is of the essence."
The findings are reported in The Journal of Clinical Investigation.