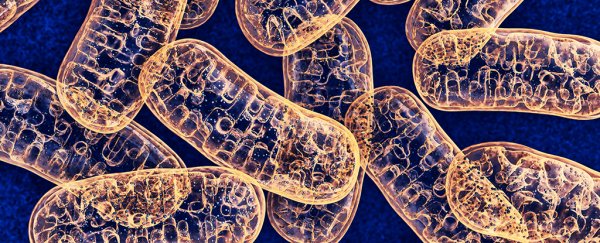
A failure to clear out dysfunctional mitochondria – the cell's energy generator – could be central to the development of the neurological disorder Alzheimer's disease, according to new research.
An international collaboration between research institutes has provided the strongest evidence yet that this shockingly common form of dementia has its roots in general cell maintenance.
"When the cleaning system does not work properly, there will be an accumulation of defective mitochondria in the brain cells," says neurologist Vilhelm Bohr from the Center for Healthy Aging and National Institutes of Health in the US.
"And this may be really dangerous."
For a disease that affects somewhere around 50 million people worldwide (a count that could potentially double in coming decades), we know surprisingly little about it.
The facts all point to a loss of brain cells in key regions of the brain as they accumulate a tangled mess of tau proteins and clumps of protein called beta amyloids. This protein dump is a death-stroke for neurons, but tracing the pathway back to a smoking gun has proven difficult.
Having certain genes raises your risk of developing the condition, as can sleep disruption, and even the presence of the herpes virus can make a difference.
Somewhere in this mix of clues there's a biochemical narrative of breakdown, loss, and eventually cell death. We're just yet to put the pieces together.
This latest study could provide fresh insight, demonstrating how an accumulation of old 'cell batteries' leads to signs and symptoms of Alzheimer's in tissue cultures and animal models.
Most types of cell in your body house numerous tiny structures called mitochondria, which turbo-charge the conversion of glucose into an energy currency called ATP.
These itty-bitty powerhouses can fail from stress or damage. When they do, they need replacing. But the old mitochondria also need to be broken down and disposed of, a process referred to as mitophagy.
The link between defective mitochondria in nerve cells and neurological diseases has been fertile ground for researchers for some time, but this is the first study to explore the role of the clearing process itself.
A close look at post-mortem samples of tissue taken from the hippocampus of deceased Alzheimer's patients showed a greater number of undersized and faulty mitochondria.
The team also noticed a large amount of AMP-activated protein kinase (AMPK), a chemical that triggers the degradation of mitochondria so they can be dismantled and removed. It was clear that in spite of this trigger taking effect, it wasn't resulting in mitophagy.
To confirm the weak links in the chain, the team created cultures of Alzheimer's brain tissue from neural stem cells and measured quantities and activity of proteins associated with mitochondria clearance.
With suspects in mind, they next turned their attention to animal models that had been tweaked to reflect Alzheimer's-like physiology and function.
The worm Caenorhabditis elegans might not initially seem like the best candidate for dementia experimentation, but its simple nervous system and ability to carry out basic memory tests have made it a suitable model in the past.
This time, the researchers not only demonstrated the significance of various proteins in locking up the mitophagy process, they were able to reverse the condition's effects.
Removing the defective mitochondria also saw the concentrations of beta amyloid plaques drop and a reduction in the chemical changes to tau proteins that cause them to tangle.
"It significantly strengthens our results that the cleaning process seems to be important in both human cells and across different animal species," says Bohr.
"And then it is encouraging that in living animals we are able to improve the central Alzheimer's symptoms, memory and learning."
As exciting as this development is, it could still be many years before we have treatments that repair the mitophagy process in humans and help our brain cells deal with their old powerhouses.
Still, every piece of the puzzle brings us closer to understanding how Alzheimer's disease develops, and potentially a way to prevent or even cure it.
This research was published in Nature Neuroscience.