Understanding the timeline of Alzheimer's degeneration can improve support for those affected, and researchers have now built a new 'molecular clock' to predict the onset of symptoms years in advance, using established blood markers.
The time between the first biological signs of Alzheimer's appearing and cognitive issues becoming noticeable can be 10–30 years in most patients, and scientists are keen to understand more about what affects that window.
The molecular clock narrows down when someone might start showing memory problems to a three or four-year window. While it's not the first predictive tool to be discovered, it may be among the simplest and quickest yet.
According to the team developing the tool, led by researchers at Washington University in St. Louis (WashU) in the US, this will be useful first for group-level studies and later for individual patients.
"Our work shows the feasibility of using blood tests, which are substantially cheaper and more accessible than brain imaging scans or spinal fluid tests, for predicting the onset of Alzheimer's symptoms," says neurologist Suzanne Schindler, from WashU.
"In the near term, these models will accelerate our research and clinical trials. Eventually, the goal is to be able to tell individual patients when they are likely to develop symptoms, which will help them and their doctors to develop a plan to prevent or slow symptoms."
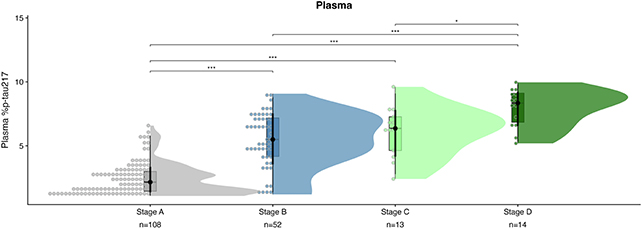
The researchers used an existing blood test that measures levels of the p-tau217 protein. This protein can already be used to diagnose Alzheimer's, but with some additional mathematical modeling, the researchers found it could also predict whether someone is likely to develop symptoms and when.
Previous studies have shown that p-tau217 in the blood is an indicator of tau and amyloid-beta protein build-up in the brain – abnormalities that are strongly associated with Alzheimer's disease and the damage it does to neurons.
The researchers analyzed existing blood test data from 603 people collected over several years to develop their Alzheimer's clock test. By looking at p-tau217 levels in the samples and when cognitive issues first appeared, the team was able to develop formulas to link the two events.
Older people tended to have a shorter window between the two points, the researchers observed, perhaps indicating that younger brains are better able to resist neurodegeneration and keep it at bay for longer, once it's begun.
"Amyloid and tau levels are similar to tree rings," says lead author and neurologist Kellen Petersen, from WashU. "If we know how many rings a tree has, we know how many years old it is."
"It turns out that amyloid and tau also accumulate in a consistent pattern and the age they become positive strongly predicts when someone is going to develop Alzheimer's symptoms. We found this is also true of plasma p-tau217, which reflects both amyloid and tau levels."
It's important to emphasize that right now, the accuracy of the test is only useful for analyzing large groups of people – it's not something that can reliably tell one person how long it will be until the symptoms of Alzheimer's start showing (though that may come in the future, with further research).
However, that still makes the blood test valuable for planning clinical trials and studies into Alzheimer's.
If researchers know roughly when memory and learning problems are going to strike in a subset of people, trials can be arranged across those years to get a close look at the progression of the disease and the associated biological changes.
Related: The Link Between Air Pollution And Alzheimer's Is Now Clearer Than Ever
"These clock models could make clinical trials more efficient by identifying individuals who are likely to develop symptoms within a certain period of time," says Petersen.
"With further refinement, these methodologies have the potential to predict symptom onset accurately enough that we could use it in individual clinical care."
The research has been published in Nature Medicine.