A discovery by researchers from the Baylor College of Medicine in the US could lead to treatments that clear the troublesome aggregations of protein thought to play a key role in Alzheimer's disease.
Using mice bred to have a condition similar to the neurodegenerative disorder, the team found that elevated levels of a protein called Sox9 triggered specialized brain cells to go into clean-up overdrive, 'vacuuming' up plaques with increased efficiency.
In behavioral and memory tests, the treated mice also performed better, suggesting that the intervention can help protect the brain and reverse cognitive decline – a process that typically occurs in Alzheimer's disease as neurons are damaged and destroyed.
Related: There's One Critical Thing You Can Do to Keep Alzheimer's Symptoms at Bay
The researchers found that the benefits of Sox9 stemmed from increased expression of a receptor called MEGF10, exclusively expressed in the membranes of brain maintenance cells called astrocytes, which are deployed to remove amyloid-beta plaques.
"Astrocytes perform diverse tasks that are essential for normal brain function, including facilitating brain communications and memory storage," says neuroscientist Dong-Joo Choi, previously at the Baylor College of Medicine and now at the University of Texas Health Science Center at Houston.
"As the brain ages, astrocytes show profound functional alterations. However, the role these alterations play in aging and neurodegeneration is not yet understood."
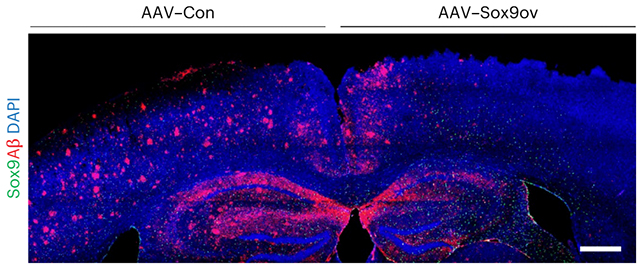
Some extra Sox9 seems to give the aging astrocytes a new lease on life, the researchers found. The Sox9 protein has previously been found elevated in Alzheimer's brains, which may indicate the brain's attempt to ramp up waste removal.
The researchers tried an opposite experiment, too, genetically engineering mice to remove Sox9. In these animals, the astrocytes showed signs of reduced health, memory recall worsened, and more amyloid-beta clumps stacked up.
"An important point of our experimental design is that we worked with mouse models of Alzheimer's disease that had already developed cognitive impairment, such as memory deficits, and had amyloid plaques in the brain," says Choi.
"We believe these models are more relevant to what we see in many patients with Alzheimer's disease symptoms than other models in which these types of experiments are conducted before the plaques form."
Scientists are now tackling the challenge of Alzheimer's disease from numerous different angles, including treatments that target amyloid-beta plaques. However, not all of these treatments work, emphasizing the complexity of the disease.
There are multiple ways to clear out amyloid-beta clumps or stop them from forming, but we're still not sure if these protein aggregations are causing Alzheimer's or just a result of the disease. All of these factors need to be weighed up by researchers.
However, each new study gets us closer to understanding how this disease progresses – and how, eventually, it might be stopped. Although these latest tests were carried out in mice rather than humans, there's good reason to believe scientists may have discovered a crucial new route to tackling the manifestations of Alzheimer's.
"Most current treatments focus on neurons or try to prevent the formation of amyloid plaques," says neuroscientist Benjamin Deneen. "This study suggests that enhancing astrocytes' natural ability to clean up could be just as important."
The research has been published in Nature Neuroscience.

