While COVID vaccines have saved millions of lives globally by reducing the overall severity of the disease, nearly one in ten of those recovered are still ending up with ongoing symptoms after the initial illness has passed.
These patients are presenting with a staggering array of over 200 symptoms, including dizziness, diarrhea, breathlessness, fatigue, and debilitating brain fog, which can linger for months or even years.
Frustratingly, even long COVID patients describing breathing-related problems are showing normal results on standard clinical breathing tests, says respirologist Michael Nicholson from St. Joseph's Health Care London.
But a new imaging technique has now clearly revealed the source of the breathing problem.
"The findings allowed us to show that there was a physiological impact on [patient] lungs that correlated with their symptoms," Nicholson says.
 (Alexander Matheson)
(Alexander Matheson)
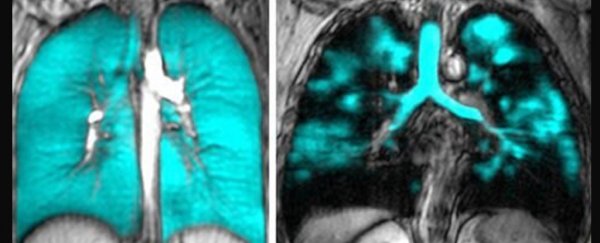
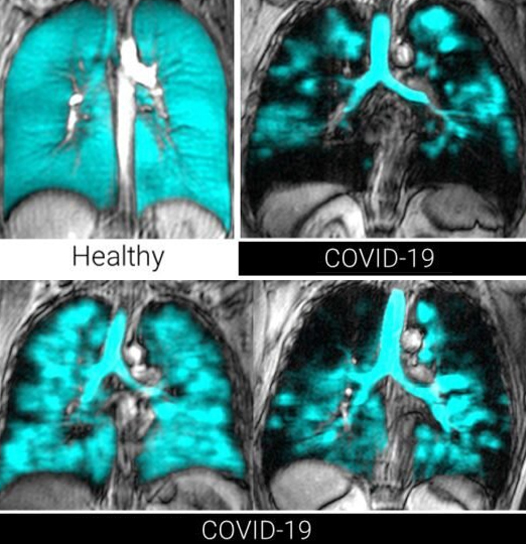
The scans demonstrate the extensive damage having COVID-19 can cause to our delicate respiratory organs. Whether it's the virus itself or the body's response to it, some mechanism has effectively pruned the function of patients' lung vessels, lopping off many of the smallest ones where the all-important gas exchange takes place.
The researchers, led by Western University physicist Alexander Matheson, instructed 40 volunteers – 34 with post-acute COVID-19-syndrome, and 6 without – to inhale a polarized xenon gas isotope. The gas resonates at a signature frequency under MRI, allowing the researchers to observe the activity of tiny airways and blood vessels in real time.
"For those who are symptomatic post-COVID, even if they hadn't had a severe enough infection to be hospitalized, we are seeing this abnormality in the exchange of oxygen across the alveolar membrane into the red blood cells," says Western University medical biophysicist Grace Parraga.
"What we saw on the MRI was that the transition of the oxygen into the red blood cells was depressed in these symptomatic patients who had had COVID-19, compared to healthy volunteers."
Because flu symptoms are the most obvious and common signs of COVID-19 it is often dismissed as just another respiratory disease, but COVID-19 is actually a vascular disease too, meaning it can interfere with the circulatory system. The virus particles directly target endothelial cells, which line the walls of our blood vessels and heart.
The vascular damage is reflected by the MRI scans; CT scans also confirm the abnormalities in the finest blood vessels in our lungs.
What's more, a previous study has already demonstrated a shift in blood distribution from smaller to larger blood vessels within the lungs of hospitalized COVID patients.
The team proposes several potential mechanisms for the alteration in gas exchange they witnessed, illustrated in the diagram below.
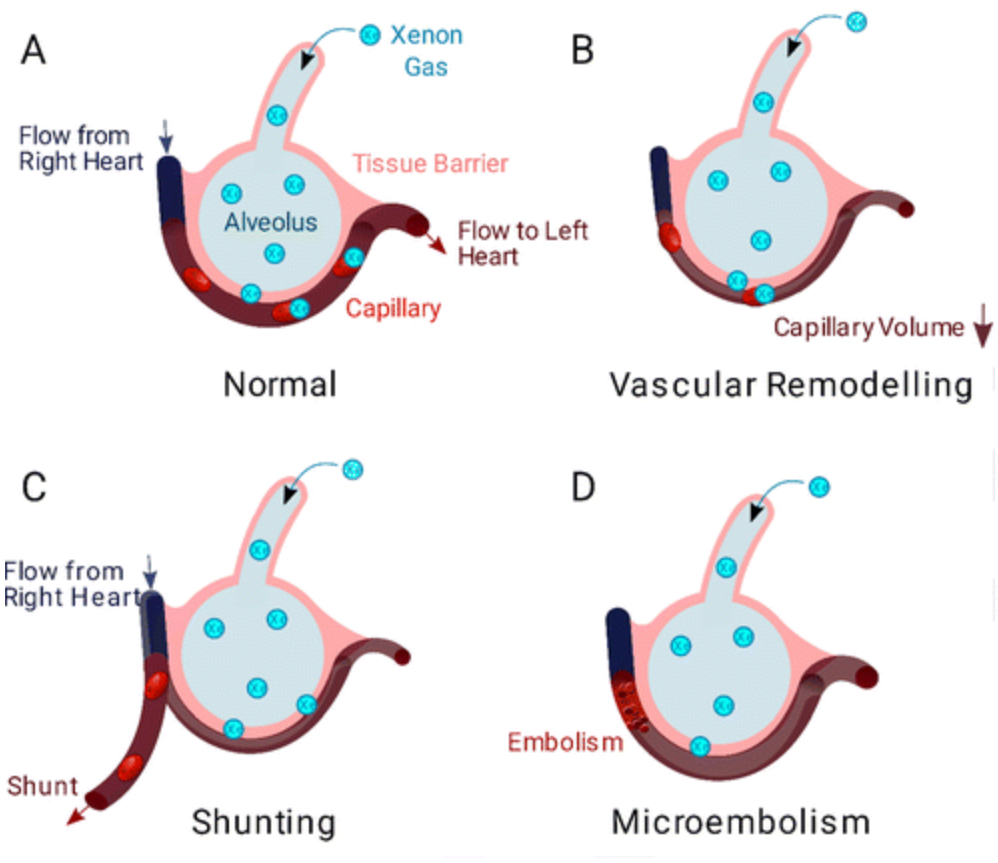 Possible mechanisms for disrupted gas exchange. (Matherson et al., Radiology, 2022)
Possible mechanisms for disrupted gas exchange. (Matherson et al., Radiology, 2022)
The vessels may be losing their flexibility which reduces how much blood is available for xenon to bind to (B), new blood flow patterns thanks to changes in vessels elsewhere may be shunting the blood away from the gas exchange regions (C), or there is a physical blockage preventing the blood from getting there (D).
Matheson and colleagues caution that the small sample size limits their ability to generalize, but urge for further investigation. And whatever the mechanism behind this is, it is starkly clear catching the virus can really mess with the circulatory system.
Despite restrictions easing in many parts of the world, the global pandemic remains ongoing, and each SARS-CoV-2 infection risks vascular damage, from clotting problems to heart disease.
"I was on oxygen for almost two months after COVID, and it took me almost three months to get to a place where I could go for a walk without gasping for air," one of the study participants, bobsled Olympic gold medalist Alex Kopacz explains.
"The take-home message for me is that we have to remember that this virus can have very serious long-term consequences, which are not trivial. In my case, prior to getting sick, I didn't think it would really affect me."
This research was published in Radiology.