The human body is sometimes said to host 'two' brains – the big one in your skull and the mini version in your gut.
The bridge between the two is known as the gut-brain connection, and in recent years, this two-way street has emerged as a promising avenue to slow the cognitive decline that often occurs as we age.
A recent review of 15 human studies, published between 2012 and 2025, has now laid out some of the strongest trials to date on the subject. Even combined, the results are preliminary, but they suggest that rebalancing the gut microbiome may prevent or mitigate cognitive decline in older adults.
The review of clinical trials covers 4,275 adult participants over the age of 45 across Europe, Asia, North America, and the Middle East, who were diagnosed with dementia, cognitive impairment, or conditions that increase the risk of cognitive decline.
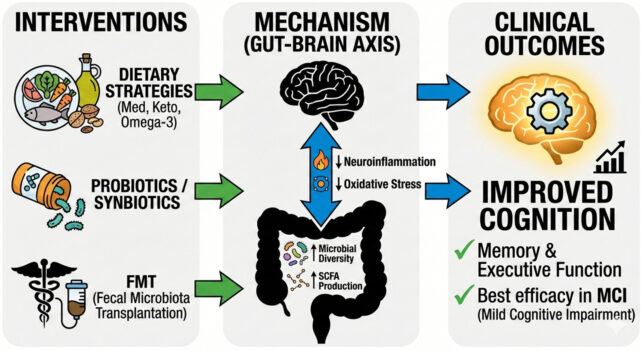
Some of these participants underwent gut microbe interventions, either through indirect dietary strategies, like the Mediterranean diet, the ketogenic diet, or omega-3 supplements, or more direct interventions, such as probiotics, prebiotics, or poop transplants.
Comparison groups received a placebo, standard care, or alternative nutritional interventions.
Overall, those who received a gut-modulating intervention showed gut microbes with greater diversity. They also showed greater improvements to memory, executive function, and global cognition. That was particularly true for individuals with early or mild cognitive impairment, but the effects were limited for advanced Alzheimer's disease.
"The reviewed interventions appear to mediate cognitive benefits by modulating the gut microbiota and its metabolic outputs," the review authors conclude, led by researchers in Italy and Spain.
The findings are promising, but longer-term randomized controlled trials are needed to determine, with greater certainty, what is happening with each intervention and why.
Fecal matter transplants are cutting-edge, largely experimental procedures, but in the review, they showed some of the most striking outcomes.
In one reviewed study, five patients with Alzheimer's who received a single transplant later showed a greater richness of gut microbes in stool samples. These five participants also showed improvements on two cognitive tests that assess memory, attention, language, and problem-solving.
"Compared with dietary or probiotic interventions, FMT appears to induce more rapid and pronounced microbial shifts, though long-term stability and safety remain uncertain," explain the review authors.
Dietary changes and nutritional supplements, by comparison, come with fewer risks, and while they may take longer to take effect, they could still be useful.
Some recent twin studies, for instance, have found that certain plant-fiber prebiotics, which promote 'good bacteria' in the gut, can boost brain function in older adults.
Other studies suggest that probiotics, which directly deliver 'good bacteria' to the gut, may help with mood disorders or stress, but rigorous clinical research remains limited.
In the current review, several small randomized trials supported the idea that probiotic and other 'synbiotic' interventions "improve executive function, memory, and verbal fluency, alongside increased microbial diversity and altered neurotransmitter pathways."
What's more, older adults on a Mediterranean diet incorporating olive oil or mixed nuts showed significantly better cognition scores compared to low-fat controls.
Why certain interventions improved the gut microbiome and brain function more than others is beyond the scope of this review, but the authors have outlined several hypotheses.
It's thought that some compounds produced by gut microbes, such as short-chain fatty acids, may have anti-inflammatory and neuroprotective effects.
Boosting beneficial gut bacteria may also help restore 'leakiness' in the intestinal barrier, which otherwise allows microbes to exit the gut, triggering inflammation as they go.
Or maybe gut microbes are affecting the immune system or sleep, two other areas closely tied to dementia.
Related: This Diet Helps Lower Dementia Risk, And We May Finally Know Why
The research is limited, but what is becoming clear is that hidden rhythms in the gut can impact the brain, and rhythms in the brain can impact the gut. Some scientists now argue that this bidirectional communication is so strong that it should be considered a distinct sense, the sixth in our species' arsenal.
Knowing more about this hidden sense would open the door to treating not just dementia, but a plethora of other health conditions.
The study was published in Nutrition Research.

