Pancreatic cancer is on course to be the second-leading cause of cancer-related death in the US by 2030, in part because 85 percent of cases aren't diagnosed until the disease has spread.
We're just not catching it early enough.
Thanks to a newly developed AI model from researchers at the Mayo Clinic and University of Texas MD Anderson Cancer Center, that might be about to change.
Their new system, called REDMOD (radiomics-based early detection model), was tested on CT scans from people later diagnosed with pancreatic cancer.
In nearly 3 out of 4 cases, REDMOD successfully spotted the most common form of pancreatic cancer around 16 months before diagnosis. That's nearly double the detection rate of specialists reviewing the scans without AI assistance.
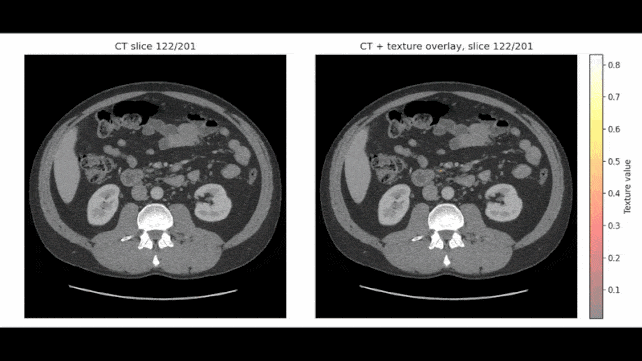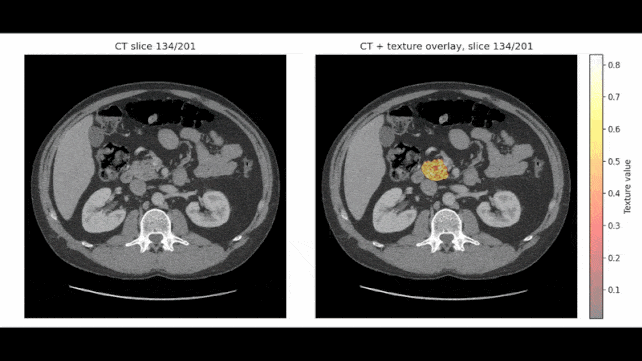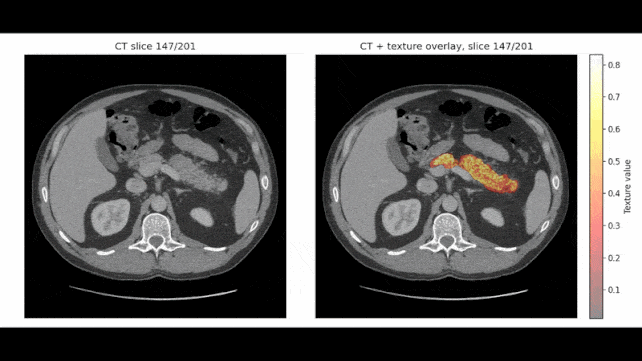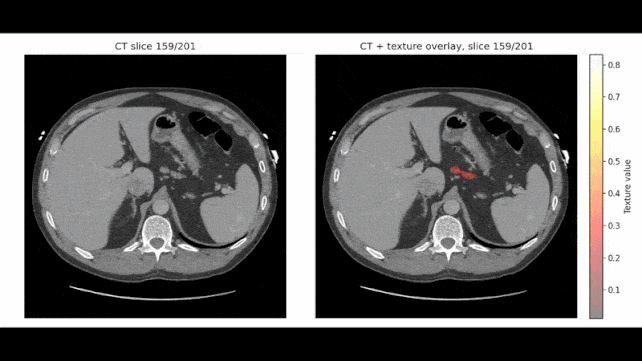
In some scans, REDMOD identified suspicious tissue patterns more than two years before diagnosis, and the team thinks it could spot cancer up to three years ahead of time.
"The greatest barrier to saving lives from pancreatic cancer has been our inability to see the disease when it is still curable," says radiologist and nuclear medicine specialist Ajit Goenka, from the Mayo Clinic.
"This AI can now identify the signature of cancer from a normal-appearing pancreas, and it can do so reliably over time and across diverse clinical settings."
The researchers used 969 CT scans of the pancreas as training data for REDMOD, so it could learn to spot the subtle signs of cancer at its earliest stages.

Rather than looking for an obvious tumor, the model searches for radiomic patterns, disruptions in tissue texture and structure that are often too minor for the human eye to spot.
Many cancers get started when normal cells acquire DNA mutations that affect how they grow and divide, but it can take years for those changes to develop into a tumor large enough to cause symptoms or appear clearly on a scan.
After the training process, REDMOD was put to the test on a different set of CT scans: 63 from people who went on to have cancer but got scanned before diagnosis, and 430 healthy controls who didn't have cancer.
Of the 63, REDMOD correctly flagged 46 as suspicious, a rate of 73 percent (almost 3 in 4).
All of these scans had previously been given the all-clear by human radiologists, and two radiologists who reviewed the scans at the same time as REDMOD identified early signs of cancer in only 38.9 percent of cases.
Of the 430 healthy controls, 81 were incorrectly identified as suspicious by REDMOD – so if the AI had been deployed in a real scenario, these people may have been called in for extra tests before being given the all clear.
A similar level of performance was shown in two other dataset tests, using different equipment at different hospitals.
Even better, for patients with multiple scans available, the AI produced largely consistent results – even when the scans were run months apart.
"These attributes position it for prospective validation in high-risk cohorts, a necessary step towards shifting the paradigm from late-stage symptomatic diagnosis to proactive pre-clinical interception," write the study authors in their published paper.
The thinking is that the earlier REDMOD can access CT scans – perhaps taken routinely for other purposes and conditions – the more useful it can be. It's possible that it could detect pancreatic cancer at a stage when curative treatment may still be possible.
There's still work to do before that can happen, though. Next, the researchers want to test the AI across larger, more diverse groups of people and see how easily doctors can incorporate it into their existing processes.
The researchers are encouraged by these early results, and hope that with further development and fine-tuning, we may have an incredibly useful system for one of the deadliest cancers around.
Related: Personalized Vaccine For 'Deadliest Major Cancer' Keeps Patients Alive 6 Years Later
"The demonstrated ability of the framework to consistently detect these occult signals on a large clinically-oriented dataset, combined with its high longitudinal stability and validated specificity, establishes a robust foundation for AI-augmented early detection," write the researchers.
The research has been published in Gut.