Diagnostic tests are continuing to get better at spotting the earliest signs of dementia, and new research suggests that a simple blood sample could help identify those at most risk, some 25 years before symptoms start showing.
Warning is crucial with conditions like dementia. It gives more time for preventative treatments to be put in place, for support and care to be prepared, and for researchers to study the biological processes involved.
In this new research, carried out by a team from institutions across the US, blood samples from 2,766 women aged between 65 and 79 were analyzed. All participants were cognitively healthy when the samples were taken in the 1990s, and their cognitive abilities were monitored over time, for up to 25 years.
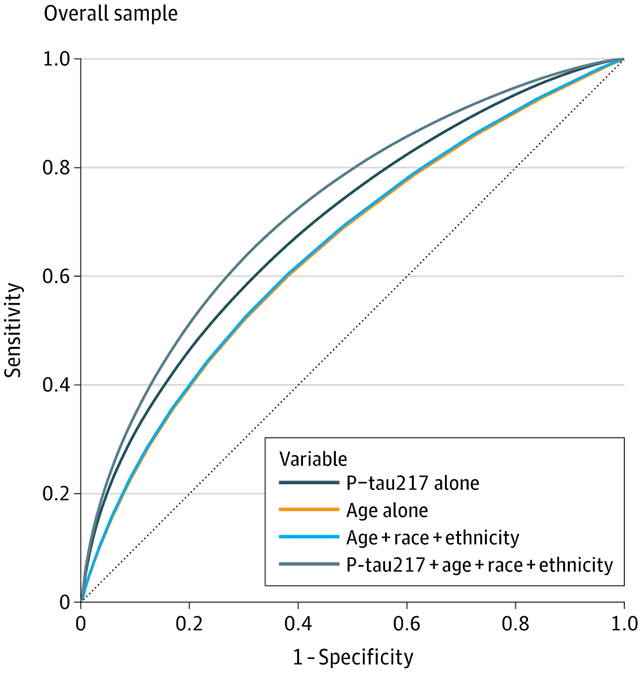
The researchers were looking for a protein in the blood called plasma phosphorylated tau 217 (p-tau217). Higher levels of these fragments in the blood have been linked to tau protein tangles in the brain, which are a hallmark of Alzheimer's and other forms of dementia.
"Blood-based biomarkers like p-tau217 are especially promising because they are far less invasive and potentially more accessible than brain imaging or spinal fluid tests," says neuroscientist Linda McEvoy, from the Kaiser Permanente Washington Health Research Institute.
"This is important for accelerating research into the factors that affect risk of dementia and for evaluating strategies that may reduce risk."
The researchers found a strong association between higher levels of p-tau217 in the blood and a higher chance of developing both mild cognitive impairment (MCI) and dementia. It's not a guarantee that someone will go on to develop dementia, but p-tau217 does seem to be a useful biomarker.
This isn't a new blood test, and it's been used in several previous studies, too. What this research adds is the unusually long follow-up time (up to 25 years) and a breakdown of the results based on race and whether or not participants had used hormone therapy.
For the hormone therapy participants, the picture was mixed. Higher p-tau217 predicted dementia clearly in women who had taken estrogen and progestin, but not estrogen alone. For MCI, there was no clear link between p-tau217 and hormone usage.
As for race, while the dementia link held for both White women and Black women, there was no association between high p-tau217 levels and MCI in Black women. The researchers suggest this might be down to misdiagnosis or because dementia may have different contributing factors in Black women.
"It is also possible that racial differences in these associations arise from differences in demographics, comorbidities, and other characteristics between Black and White women that we could not fully control for and from the lower sample size in Black compared with White women," write the researchers in their published paper.
The connection between higher p-tau217 and dementia was stronger in women over 70, the researchers also found, and in those carrying the APOE ε4 gene that has been linked to Alzheimer's disease in the past.
Related: Brain 'Stretching' Is The Secret to Protecting Your Mind From Dementia
While the p-tau217 blood test isn't yet ready for screening the general public – more research will be required before that happens – the results in this latest study take us another step forward in understanding how Alzheimer's and dementia in general get started, and how they might be stopped.
"These results add further support for growing evidence that testing p-tau 217 in blood might be an important way to screen for people who are most at risk of dementia, years before a diagnosis is made," says University of Oxford neurologist Masud Husain, who wasn't involved in the research.
As the data shows, high levels of p-tau217 don't always lead to dementia, even though tau-related brain changes are likely to have already started. The exact reasons for that could be one avenue for future studies to explore.
"Our study suggests we may be able to identify women at elevated risk for dementia decades before symptoms emerge," says epidemiologist Aladdin Shadyab, from the University of California, San Diego.
"That kind of long lead time opens the door to earlier prevention strategies and more targeted monitoring, rather than waiting until memory problems are already affecting daily life."
The research has been published in JAMA Network Open.