Research has shown that living at higher altitudes lowers your risk of developing diabetes, but scientists haven't been able to pin down why that is – until now.
A new study on mouse models of type 1 and type 2 diabetes, by researchers in the US, has found that as altitude increases and the air gets thinner, red blood cells become sponges for glucose, lowering blood sugar levels.
Under conditions of chronic low oxygen in the inhaled air, red blood cells showed a threefold increase in glucose uptake.
This metabolic shift helps cells deliver oxygen more efficiently when oxygen is scarce, the scientists explain, but it also means blood sugar is better regulated – and diabetes becomes less likely.
While it's still early days in figuring out how this new knowledge could be helpful to humans, with further research and testing, this natural management method might be adapted into treatments to prevent or reverse diabetes.
"Red blood cells represent a hidden compartment of glucose metabolism that has not been appreciated until now," says biochemist Isha Jain from Gladstone Institutes, an independent, nonprofit research organization.
"This discovery could open up entirely new ways to think about controlling blood sugar."
It's well established that living at higher altitudes changes the body in numerous ways, as it adapts to the different pressures of the environment. However, knowing exactly what's changing and why can be a challenge.
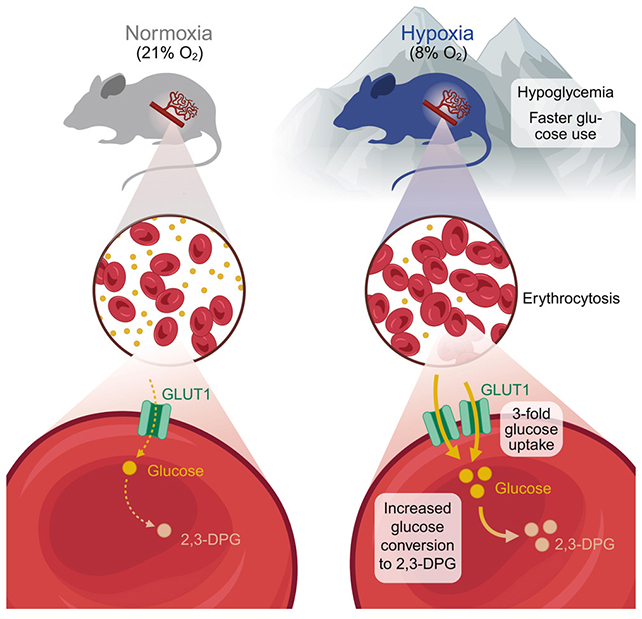
These new findings are based on experiments in mice exposed to low-oxygen environments, inducing hypoxia. To begin with, the researchers saw that the animals had lower-than-normal blood glucose levels – but it wasn't clear where the sugar was going.
Any sugar given to the mice disappeared from the bloodstream almost instantly, thereby lowering the risk of diabetes. However, it hadn't been sent to any of the expected places – including the muscle, brain, or liver. What's more, the effect lasted for weeks after the mice returned to normal oxygen environments.
By switching imaging techniques and running follow-up tests, the research team discovered that red blood cells had previously hidden talents as glucose absorbers and were responsible for efficient blood sugar regulation.
One particular molecule was identified that made the difference, acting on hemoglobin – the oxygen-carrying protein in red blood cells – and loosening its grip on oxygen, improving its circulation around tissues.
"What surprised me most was the magnitude of the effect," says biochemist Angelo D'Alessandro, from the University of Colorado.
"Red blood cells are usually thought of as passive oxygen carriers. Yet, we found that they can account for a substantial fraction of whole-body glucose consumption, especially under hypoxia."
It's a promising new finding, although researchers will need to test their discoveries outside of mouse experiments to confirm what's happening. This also aligns with earlier studies showing how red blood cells adapt to low-oxygen environments.
That other animals also show the same sort of mechanisms for glucose management at high altitudes suggests that this capability has evolved across species to improve metabolic efficiency when oxygen is scarce.
Encouragingly, by giving mouse models of type 1 and type 2 diabetes a newly developed drug that mimics the effects of high-altitude living, the researchers reversed high blood sugar levels in the animals – suggesting a treatment developed along these lines could eventually tackle diabetes.
Related: Gestational Diabetes in US Surges by 36 Percent Over Last Decade
That's probably a long way off, but there are lots of different research routes that can be taken next. These findings might also be useful for studying other aspects of hypoxia and the adaptations it induces.
It also helps explain why Sherpas have typically not shown the lower blood sugar levels found in other people living at high altitude: It could well be because of genetic adaptations preventing them from producing more of the 'glucose sponge' red blood cells observed in this study.
"This is just the beginning," says Jain. "There's still so much to learn about how the whole body adapts to changes in oxygen, and how we could leverage these mechanisms to treat a range of conditions."
The research has been published in Cell Metabolism.

